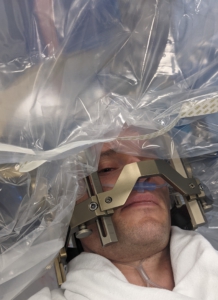
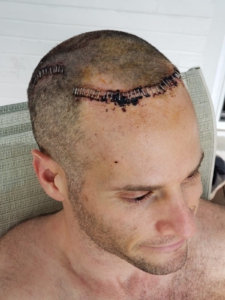
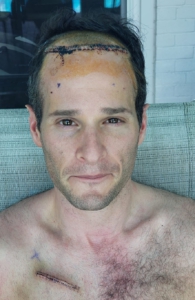
A picture of Benjamin undergoing DBS.
Benjamin after he underwent DBS surgery on June 2nd, 2021
Five days after surgery: “Bandages off and feeling good. Back home for at least the next month or so with one goal – do nothing, just lie around and let the body heal.”
#12: Benjamin Stecher – A personal account of Parkinson’s and Deep Brain Stimulation
Benjamin Stecher is doing impressive work in is role a scientific writer and patient advocate. He co-authored the book “Brain Fables” together with Alberto Espay, which recently won the prose award by the Association of American Publishers in the category Neuroscience. The book is truly unique in its way to combine both the views of patient and health professional on the history and misconceptions of Parkinson’s Disease and what should change in our field to make progress.
Benjamin was diagnosed with Parkinson’s disease at 29. Since then, he left a successful managing partner position in Shanghai to study the disease full time. He has been traveling the world to witness the latest and greatest progress being made in over 100 research laboratories around the globe. He has interviewed over 80 international experts and shares his insights on the website tmrwedition.com.
On June 2nd, Benjamin underwent deep brain stimulation surgery to the subthalamic nucleus. We are incredibly grateful that a mere nine days after that, he shares this experience lived from the most direct and intimate, the most important perspective: the one of the patient.
Benjamin Stecher 00:00Knowing that I might be able to jump in that time machine and go back to where I was five, six, seven years ago, it's liberating. You said, I think you used the right word. It's a very liberating experience. And I'm a little afraid, to be honest, of what I'm going to do with that newfound freedom. Because I've always been very spontaneous. I've always been kind of an impulsive kid. And this was long before I started the dopamine agonist, so it has nothing to do with my medication. But I'm a little worried about what I'm going to do. If and when the stimulation gets turned on and I start reaping all the benefits from this. Because Parkinson's has taken away my freedom. It's taken away my liberty. It's taken away my ability to do the things that I want to do with my day. If suddenly, at the flick of a switch, that gets restored, I have no idea how I'm going to react. I have no idea what I'm going to do. I hope to be as present in that moment as I possibly can be. But suffice to say, it's something I'm deeply looking forward to. Welcome to Stimulating Brains.
Andreas Horn 01:16Hello and welcome to Stimulating Brains, everyone. Once more, this is episode number 12. And I'm really excited about this episode. When I started the podcast, I'm told, colleagues about it in the very beginning, a lot of people told me this could also be a great way to integrate the views of patients and other healthcare professionals in this show. And I've been following the work of Benjamin Stecher for quite a while now. He's doing an amazing job in scientific outreach, scientific communication. And he is a patient advocate for Parkinson's disease because he has been diagnosed with early-onset Parkinson's disease at the age of 18. He's also a consultant for the 02:07I believe the name is a bit off the top, but anyway, Benjamin wrote the book Brain Fables together with the international expert, Alberto Espay from Cincinnati, which I can really recommend. And it's a beautiful book, combining the views of the medical doctor and the patient in the same book. When Benjamin wrote on his blog about his upcoming DBS surgery, I thought to finally reach out to him. And indeed, he was happy to join the show. And he then tweeted about the DBS surgery. And it was quite amazing already to see this procedure that I've been following along from the other side for around seven years now from the patient perspective. Now, I told Benjamin to reach out to me whenever he was ready. There was no hurry, of course. 03:01And surprisingly, he already reached out nine days after the surgery. So, yeah, I'm really happy about this. And the plan is to repeat the conversation one more time once DBS is switched on so that Benjamin can tell us a bit more about how his path continues. So thanks so much for tuning in. And I'm pretty sure you'll enjoy as much as I did. The conversation I had with Benjamin Stecher about his very own deep brain stimulation surgery. So thank you so much for taking the time, Ben, to break the ice. One thing I always ask as a first question is, what do you do in your free time? Like when not thinking, let's say, about Parkinson's disease and not writing books. I read that you like the German TV series Dark.
Benjamin Stecher And I'm a big fan. I'm a big fan myself. That's cool. I also saw something about cryptocurrency on your website.
Andreas Horn What are your hobbies? 04:00Yeah. Yeah, I love the show Dark.
Benjamin Stecher It's probably the biggest of everything I've watched over the past couple of years. No story has captivated me as much as that show. It's really a unique way of telling the story. I love the devices used. I love everything about it. When I'm not thinking about Parkinson's or I'm not thinking about advocacy or I'm not writing, I like to play and watch basketball. And I like to play and watch basketball. I'm a big fan of the NBA. I like to swim. Oh, I liked to swim, I guess. It might be a while before I can do that now. But I'm, you know, you have to make some sacrifices along the way. Sure. And I like to play golf. I like to be outside. I like to play tennis as well. I like to be active. I like to try to run around as much as I can.
Andreas Horn And yeah, other than that, I like to read.
Benjamin Stecher I have a pretty wide variety of interests. And what I read, a pretty eclectic mix there. And travel. That's probably my biggest drug, other than the drugs that I take, is getting out and seeing the world. 05:06Great. Great. Sounds amazing. So lots of things to do. Now, diving into it. So I think we are around the same age, the two of us. But in 2013, you were then 29 years old. Life took a different turn for you. Back then you worked on a management position in Shanghai, as I've read, and were then diagnosed with early onset Parkinson's disease.
Andreas Horn Can you talk a bit about that period of your life?
Benjamin Stecher Sure. So at the time I was riding pretty high. I was doing really well in Shanghai, managing that company that you mentioned. I was also traveling all around China, getting to see the people, getting to see my clients all over the place. I was helping expand my business. I was helping expand my business. I was helping expand to offices in Hong Kong and to Shenzhen and to other cities around the eastern coast of China. And then I got hit with that diagnosis. 06:01Now at first, it didn't concern me very much, to be honest, because I didn't understand what this disease was. I had no reference points other than Muhammad Ali and Michael J. Fox. And at the time, my symptoms weren't that bad either. So I thought, okay, if this is what Parkinson's disease is, then I can manage with this. It's not that bad. But then slowly I started to learn a little bit more. I started to delve into the research. I started to ask a lot of questions. I started to read as much as I could about this disease. And for lack of a better term, I started to realize how much trouble I was in. So I decided when I was 32 to pack up my things in Shanghai and move back to Canada to tackle this thing full time. And since then, I've been traveling around the world, visiting as many centers as I could. I probably visited over 100 different biotech or academic centers. At this point, just trying to figure out what the latest and greatest in this disease is and what the future is going to look like in terms of new therapies in the pipeline. 07:01Great. I found this nice brief bio of yours on the website of the Journal of Parkinson's Disease, which even brings us a bit beyond that. It said Benjamin Stecher was born in Nairobi, Kenya, as an Israeli to Jewish parents from Poland, but grew up just outside Toronto, Canada. He studied history and philosophy at the University of Guelph. But as soon as he got his BA, he took off and went to live and work as a teacher in South Korea for nearly three years while traveling the world. He moved to Shanghai, China at 26, spending one year at Jiao Tong University in a Chinese language program before being hired by a Chinese education company, San Li. That's what we talked about. He rose quickly and became a managing partner, where his duties included and so on and so forth. So, yeah. So, it seems like you've seen a lot of the world already. Now you travel the world to see the institutes of Parkinson's disease.
Andreas Horn I wanted to ask, do you miss traveling?
Benjamin Stecher 08:00But it seems like you travel a lot nonetheless. That's great.
Andreas Horn Yeah, I do miss traveling.
Benjamin Stecher In this past year and a half, I've been cooped up because of the pandemic. It's been difficult. It's probably the longest I've ever spent in one place in my entire life.
Andreas Horn Yeah, I miss it dearly.
Benjamin Stecher I can't wait to go out to the world again. I hope that it can open up as soon as possible. And you took on, as you mentioned, the mission to find out as much about PD than you could. You also co-founded the Parkinson's Research Advocacy Group and are a patient advisor to the World Parkinson's Congress. You not only visited so many institutes, but on your website, we can see that you also interviewed over 80 world experts in the field to date. And many of these interviews you make openly available on your website. The Tomorrow Edition, to which, of course, I'll link in the show notes. So you've interviewed experts, but today you are the expert because I'm interviewing you and you are one of us to have actually witnessed Parkinson's disease as close as very few of us as a patient. 09:09Actually experiencing bradykinesia, tremor, and rigidity in embodied form. I'm now making this sound a bit... I'm not sure if I'm making this sound as good as it was a good thing and must emphasize that, of course, it's not.
Andreas Horn But still, your insights are unique when seen from a purely scientific perspective. So would you be able to share some of them with us? How did being a patient inform your research on the topic? Yeah, so it's hard because you walk a tightrope as a patient, especially as a patient advocate or patient researcher.
Benjamin Stecher You're constantly balancing what you're reading about with what you're experiencing. And it's kind of a difficult mind game to play because you want to make sure that you're not biased by your own experience so you can look at what you're studying objectively. And that's hard because, I mean, you see the word tremor, you see the word bradykinesia, and it has a different connotation in me than it would in somebody who doesn't have this disease. 10:06And that's just a natural byproduct, I think, of being human. I have a very different relationship with those words than a researcher would. I also understand that I'm biased. And this is something that's hard as a patient advocate and something that a lot of patient advocates face, is making sure that they don't see themselves in the disease too much. So if you're going to be advocating for a disease, especially one as heterogeneous as Parkinson's, you have to remember that each person who has this disease experiences it in a very different way. You mentioned the World Parkinson's Congress. I went to the first one. I went to the second one. I went to the first one in Portland. My first experience was in Portland in 2016. There were at least a thousand patients in attendance. And you walk the halls of that giant conference center, and you look at them, and you see basically a thousand different diseases.
Andreas Horn I don't think any two patients at that conference presented their symptoms in exactly the same way.
Benjamin Stecher 11:03And that makes this disease, one, a fascinating peculiarity for researchers and for me as well, and two, it makes it extremely difficult to study. Because we have this label that we call Parkinson's, and we assign it to everybody who has this disease.
Andreas Horn But the reality is that it's, yeah, to quote Bas Bloem, there's seven million different people living with Parkinson's, living with the label called Parkinson's disease.
Benjamin Stecher Unfortunately, that might mean there's seven million different forms of this disease that we might have to tackle. That's a great quote. And it's a perfect setup for the world. And it's a perfect setup for the next question. You co-wrote a book with Alberto Espay, who is, of course, an internationally known Parkinson's disease expert in Cincinnati. The book is called Brain Fables, and it won the PROSE Award of the Association of American Publishers in the category Neuroscience this year. 12:01Congratulations for that. Let's dive into maybe very briefly what the book is about as a summary, because I think that's exactly what you just talked about.
Andreas Horn Yeah.
Benjamin Stecher So, the book is about Parkinson's disease. And it's really the idea, and to quote Alberto at this point, we've learned a lot about Parkinson's disease, but we know next to nothing about any individual living with Parkinson's disease. And I see this all the time on the various committees and various panels that I'm part of. Everyone talks about Parkinson's, especially researchers, in these generic terms. They paint with a very wide brush. And yet, when you drill down into the individuals that live with this disease, like I said before, you see so many different forms of Parkinson's. You see so many different flavors, so many different spices, so many different forms of this disease. Even the tremor that I experience.
Andreas Horn Yeah. I don't think other patients experience it exactly the same way that I experience it.
Benjamin Stecher Because mine travels from my, right now you can't see it, but it's in my left foot and it's in my right hand. I don't know anyone who has quite that same, like, that it's localized in those exact same ways. 13:07And that individual nature of this disease is very different.
Andreas Horn Yeah.
Benjamin Stecher And that individual nature of this disease makes any study of this very difficult and very challenging. But, as the book illustrates, that's the path we need to be walking. That's where we need to be heading if we're going to ever properly manage and tackle this disease. We need therapies and interventions that are not one size fits all.
Andreas Horn Yeah.
Benjamin Stecher They can each be tailored to each individual's needs at any given moment and any given time. Which is why, and I'm assuming we're going to talk about this at some point, jumping ahead a little bit,
Andreas Horn which is why I'm so excited about this new thing I have in my brain. Yes.
Benjamin Stecher That's the main topic, definitely. Very briefly, you also, like, especially I think in the beginning of the book, you wrote some chapters about the patient perspective.
Andreas Horn And there you wrote, for example, I soon realized I had more resources at my disposal than any king or emperor had ever dreamed of. 14:02How was it like to be able to speak with experts just such as John Hardy, Alfonso Fasano, and so on?
Benjamin Stecher John Hardy, Alfonso Fasano, Anatol Kreitzer, Bas Bloem, Tony Lang, but also the general neuroscience experts such as Eric Kandel or Christof Koch.
Andreas Horn How is it to have Google and PubMed to find out as many things as you could imagine about the brain and Parkinson's disease? Yeah.
Benjamin Stecher I often think of myself as being very fortunate and very lucky. Very lucky that I'm growing up where I'm growing up, here in Toronto, and I have access to the great surgeons and the great team here in Toronto.
Andreas Horn Yeah.
Benjamin Stecher And I'm very lucky to be living in the time that I'm living in. If I had been born in any other century, or even in any other decade really in the past, I would not have had the ability to access all of these great minds and all these great institutions and all this great learning that I have today. And that really has, it's allowed me, while this disease sucks and nobody would ever want it, it gives some credence to the often heard quote, now is the best time in history to live with Parkinson's. 15:06to live with Parkinson's disease. And that's very much true. And that makes me feel very fortunate and very grateful to be alive when and where I am. Great. I think you wrote Parkinson's sucks but I wouldn't trade these last few years for anything Is that still true? Yes it is. It's even more true now after the surgery to be honest.
Andreas Horn Yeah, it's given me insights into my own brain and to the human mind.
Benjamin Stecher I think that very few people can access that very few people will ever get to I mean great how many people have heard the sound of their own subthalamic nucleus. Yes, that's true. I even wanted to ask you that how was that feeling like to listen to that it was surreal uh it's something that words probably can't properly describe um to hear that static static is probably the wrong 16:03word but like it does sound like a Geiger counter of sorts um but yeah it was just surreal it was surreal to feel the whole thing it was surreal from every moment I remember very vividly every single detail of those three hours they're indelibly edged in my brain uh I hope soon to be able to write about everything so that I can get everything down on paper yeah before we get into that I think um maybe before the surgery regarding therapeutic options um that are out there uh you wrote in the book I have swallowed tablets of bear bile drank elixirs containing seal penis had bags of glutathione dripped into my veins and applied topical creams made from bird saliva moreover you considered bee sting therapy ice water immersion conscious walking electric stimulation mats high dose thiamine injections hypnosis vagal nerve vibration therapy antifungal creams and many more so so I I 17:03I work in in DBS and Parkinson's disease but I didn't even know these things existed how is it possible to navigate between truth and myth as a patient so you hit on what it what is
Andreas Horn exactly the main challenge that I faced and the big reason why I wrote this book
Benjamin Stecher Um, the original title is Brain Fictions, actually, but because our editors thought that having that would uh conflict with the non-fiction genre of writing but anyways um
Andreas Horn 18:03what are the reasons for why I trust this source over that source or why I have more faith in this hypothesis over that hypothesis.
Benjamin Stecher But really, it's been bred out of trial and error. I've tried so many things along the way. I've tried so many different kinds of therapies. At the beginning, I was very naive about everything.
Andreas Horn I thought, yeah, I believe that a lot of these therapies would work for me.
Benjamin Stecher And that belief is powerful in and of itself. Obviously, we know a lot about the placebo effect and everything that the placebo effect can do for a person. But belief is a powerful thing. If you believe something works, it has a stranglehold over you in some sense. And I see this time and time again in the news and time and time again in the patient advocacy groups that I'm a part of. That belief that something works is such a powerful magnet. It's such a powerful motivator. It's such a powerful way of getting people to do something. 19:01And yet, we think about it. We have to be grounded in reality. And knowing the difference between what is real and what is not real is the real challenge of our times, I think. We're inundated with so much information these days. There's so much resources out there. If I do a search for Parkinson's disease therapies, I can come up with probably a billion different hits that will come up. Knowing how to navigate all of that, knowing how to discern what is worth pursuing and what is not worth pursuing is the greatest challenge that I've had. Knowing how to navigate all of that, knowing how to discern what is worth pursuing and what is not worth pursuing is the greatest challenge that I've had. Knowing how to navigate all of that, knowing how to discern what is worth pursuing and what is not worth pursuing is the greatest challenge that I've had. It's the greatest challenge I feel like we face going forward in terms of properly dealing with this. And it's something that I continue to think about. Even now, after having DBS, I still wonder if I made the right decision. There's so many different options I could have pursued. There's so many different avenues I could have explored. There's so many different therapies that sound promising.
Andreas Horn Knowing, yeah, trying to hone in on which one is the right one for you as an individual is a very difficult decision.
Benjamin Stecher 20:01And frankly, I think... I think patients are in many ways left to their own devices to sort that out. There's no guidebook for what's best for you as an individual. Life doesn't come with a manual. You have to figure out the tools needed to be able to discern for yourself along the way what is the right path to take and what is the wrong path to take.
Andreas Horn How did you decide to do DBS?
Benjamin Stecher You wrote a blog post about the pros and cons of DBS, but also cell replacement therapy, focused ultrasound, and gene therapy.
Andreas Horn Why DBS in the end?
Benjamin Stecher For a number of reasons. One, I had access to a great number of experts here at the Toronto Western Hospital who have made a living or have made a career out of advancing and pursuing DBS therapies. So that was one key factor that I had the expertise in my corner. And also, in some ways I was driven by faith as well. So about three or four years ago, I was in a hospital. 21:01I was in a hospital. Two years ago, I was sitting in Hadassah Medical Center. Hadassah is a medical center in Jerusalem.
Andreas Horn Yeah.
Benjamin Stecher I was in Hagai Bergman's office. I spent with him about four hours one-on-one. He gave me like a private lecture for about four hours on closed-loop deep brain stimulation therapy. Nice. I had no idea at the time that he was basically painting my future. He was painting the future that I was going to experience. He illustrated... I didn't understand everything he said. he said and to date I don't remember everything that he said but I was profoundly impacted by that by those few hours and I didn't realize it at the time but I now know that that future that he was envisioning was the right one for me it also coalesced around another person which was Alfonso Fasano about five years ago uh what or yeah five years when I came back from China to uh pursue this 22:02full-time I started to look around at the different uh neurologists in Toronto that I had access to I would send I sent a bunch of emails to them uh asking them questions one person a couple people responded but one person really took up really took a strong interest in my case and that was Alfonso. I think I was a little bit more of a fan of Alfonso Fasano than I was of Alfonso Fasano I then went to his office I sat with him and we started to discuss this disease and my potential future therapies and I think he could see how curious I was he could see the passion I had in me to learn as much as possible and at the time I was asking some very very very simple very basic questions what is an axon what is dopamine what are neurotransmitters. I was amazed by how patient both Hagai and Alfonso were. I was really amazed and this is something I would love I hope all scientists realize the power that they have in this sense I was taken aback and I was amazed by how much time they spent just 23:05explaining those basic concepts to me um really spending the time to get to allow another person to understand what you're working on especially something that's so personal to them it was a life changer for me it was a life changer in many different ways uh but all of those things kind of came together and coalesced to bring me to where I am today All those happenstance occurrences. I've never actually spoken with Hagai Bergman since then but I remember that those three hours that I spent with him very clear four hours I spent with him very very very clearly we were it was it was yeah it was a remarkable journey that
Andreas Horn he took me on um so yeah that to make a long story short that was another reason why I chose DBS and
Benjamin Stecher then on top of it the other therapies that were options for me stem cell therapy gene therapy focus ultrasound and another one would have been um the uh subcutaneous pumps subcutaneous 24:07levodopa pumps none of them offered the uh the the none of them had the same kind of uh track record as DBS did so DBS obviously has 20 plus years of uh use in humans we have had over by last count I saw over 150 000 people have been had deep brain stimulation surgery um we've seen its successes we've know we know pretty well what it can do and what it can't do for some of these other therapies we're much more in the dark we don't have the same depth of history that we can draw upon make sense and then the final thing was just talking to patients talking to patients who have gone through this before um DBS is a very scary thing um it's a very traumatic thing to go through especially the way I chose to do it which was to be awake through the whole process but in speaking to 25:05the people that had gone through before me I was very reassured by how it's hard to say because you don't want to put the cart before the horse I'm only a week and a half out of the surgery myself I don't know if what kind of benefit I'm going to experience I don't know how successful it is for me but if I can get even half of the benefit that some of the other patients have gotten before me and some of the what we think it might do for me then I'll be happy especially because, and sorry, one other factor: my symptoms, my symptomatology in particular, and my relatively young age I think make me a perfect candidate for DBS um that is true yeah now let's talk about it um but I wanted to briefly formally say that one more time nine days ago you underwent DBS surgery 26:00to the subthalamic nucleus at the Toronto Western Hospital so it's amazing that you do this right
Andreas Horn now with me thank you so much one more time how do you feel I don't feel like somebody who's had
Benjamin Stecher brain surgery nine days ago I'll say that to begin with uh I feel surprisingly good even though it looks a little bit horrific there's a lot of crusted blood that I'm not allowed to touch um I feel very good I feel almost as good as I did uh prior to the surgery I would say at this point how was the surgery itself um you already mentioned it was awake. So depending on the hospital, people can choose, I guess, awake versus asleep surgery um or even hybrid forms so this involves mounting a stereotactic frame on your skull drilling burr holes into your skull while you're awake and then recording brain activity from microelectrodes as well as test
Andreas Horn stimulations at the target site. How was that? Yeah, that's a big question. It's unfortunately not
Benjamin Stecher 27:03something I can wrap up in a few words like I said before those three or four hours that I spent in the O.R they're indelibly etched to my brain I remember so many details from that surgery so many details from that day it's hard to put it all into words but I guess to begin with I'll by saying going into the surgery I felt very ready I felt very at peace with the decision I made I felt very good about the things going forward and this is something I wanted to emphasize quite a bit it's very hard to prepare somebody to go through something like this it's a very like I said a very traumatic thing to experience in the nine days since I've been speaking to a couple patients who are scheduled to get DBS in the coming days months and weeks some of them I see a lot of fear a lot of apprehension about what they're about to experience and I think rightfully so getting holes drilled in your brain is not a minor thing it's something that will change your 28:05life forever for good or for bad whatever happens I know I know for myself whatever happens going forward my life will change going forward, my life won't be the same. I hope for the better. I hope I'll get that maximum benefit from all this, everything that I went through, but you never know what's going to happen. You never know what the future is going to hold. So thinking back to that day, what it was like, I don't know. I don't want to describe it as a religious experience, but in some ways, it bears some similarities. Maybe mystical. It is very mystical. I remember, for example, probably the most traumatic event of the whole day, probably the most traumatic thing I went through. So the most painful parts was actually just the freezing of the scalp, when they freeze
Andreas Horn all of the different things. Yeah, they stick like at least a dozen needles in you just to freeze
Benjamin Stecher all of the areas around the skin, so you don't feel anything. After that point, you're not in 29:02pain at all anymore. So there's no pain experience. After that freezing point. But you know everything that's happening. You feel everything that's happening. And me being uber curious, I asked my neurosurgeon to explain everything that he was doing and to teach me as much as he could along the way. And there was a couple of times where he had to tell me to shut up, to stop talking, to stop asking questions because they
Andreas Horn needed to focus and they needed to concentrate, rightfully so. But yeah,
Benjamin Stecher I was there and present throughout the whole thing. I guess the most shocking part of the whole thing was the drilling of the burr holes through the skull. It was the loudest sound I've ever experienced. It was the most, the world was shaking all around me. Like the entire universe
Andreas Horn felt like it was shaking. It was something, yeah, getting holes drilled through your skull. 30:00The acoustic transmission is via the bones as well, right? So that's,
Benjamin Stecher I guess it's loud. It's loud itself, but it's much louder for you even more. Yeah. Every little scrape, every little, even though it goes, it kind of goes by in an instant, it goes by very relatively quickly. And again, there's no pain involved at all. That sound is something I'll never forget. That sound is something I'll never,
Andreas Horn yeah, I'll never be able to get out of my head. And then again, it's so hard to put everything
Benjamin Stecher into a few words or a few sentences. There's just moments that stick out. There's moments that um, make me, give me pause. It's something I'm still reflecting on, to be honest. It's something that I probably haven't completely absorbed the whole experience myself yet. It's something I need to reflect on more. It's something I'm definitely going to be writing about in the future, but it was unique. It was traumatic. It was, it made me feel alive. It was, it was horrible in some points. It was 31:00very uncomfortable, but I'm, oddly happy that I went through it.
Andreas Horn What else happened during surgery? Was there some research involved or recordings or stimulations?
Benjamin Stecher Yes. So during the surgery itself, I had a microelectrode recording of my subthalamic nucleus, and that was wild itself to hear the sound of the microphone dropping through the different layers of the cortex and then going down into the basal ganglia. And then that, that sound that you get when you hit that sweet spot of the STN and that, that pitch perfect noise that it makes. Once it hits that sweet spot was yeah. It was, it was quite remarkable just to, just to hear that sound emitting from your own brain and knowing that that electrical activity that's responsible for everything I touch and feel and experience in the world is,
Andreas Horn is remarkable in and of itself. Again, a lot of these things, I'm finding it hard to find the words, to be honest. It's the brain listening to itself, right? It's even for us outsiders standing
Benjamin Stecher 32:03by. Each time I've done this since seven years, at least to attend surgeries. And it's still remarkable to listen to the live cells firing of a living human brain. But if it's your own brain, I guess that's a whole different story. It is. It is a whole different story. I wonder, I remember, I remember thinking very vividly at that time. So I was tapping my fingers together. I was trying to manipulate the sound. I was trying
Andreas Horn to manipulate what was happening.
Benjamin Stecher And I couldn't, I don't know if I was successful in being able to do so in real time. But that idea that that thought that that electrical current that gave rise to that noise that allowed me to do this was yeah. Trying to tweak that in real time was a pretty crazy experience. And then on top of that. 33:00So then once the stimulation was turned on. So once I started to feel that. I started to feel some of the symptomatic benefit. That's when I knew that.
Andreas Horn Again, I don't know how to put this into words exactly. But so right now I'm off. This is what you're seeing
Benjamin Stecher the camera. This is what I experienced when I'm off. I'm stiff, I have a tremor. It's hard for me to move about properly. When you turn on the stimulation, and suddenly I could move my wrist and my hand and my arms. It was like taking a time machine back in time. To when I was years ago, soon after my diagnosis when I felt pretty good. I felt good. I didn't need any medication really at the time. Jumping back in time like that just by that stimulating that part of my brain. Again, it's hard to put into words what
Andreas Horn is it liberating? I could imagine that because you suddenly are able to move more again.
Benjamin Stecher 34:01liberating is a good way of putting it I would say.
Andreas Horn Yeah, I would say part of it is liberating. Yeah, I would say part of it is liberating. move about fairly comfortably in the world. I no longer felt those, yeah, it was almost like being
Benjamin Stecher freed from jail. You feel just that release, that easing of the tension and that all the anxiety, all the stress of having this disease, of having to manage it day in, day out.
Andreas Horn It kind of dissipates. It all goes away. Yeah, because one thing about Parkinson's, it's a very
Benjamin Stecher 35:01stressful way to live a life simply because everything is so unpredictable. You can't predict when you're going to be on, when you're going to be off, when you're going to be dyskinetic, when you're going to be bradykinetic, when you're going to be, when you're going to feel a tremor, when you're going to feel dystonia. It's very difficult to plan your days. Knowing now that it's possible that I might be able to, once the programming begins and once I find the right settings for myself, knowing that I might be able to jump in that time machine and go back to where I was Five, six, seven years ago. It's liberated. You said, I think you used the right word. It's a very liberating experience. And I'm a little afraid, to be honest, of what I'm going to do with that newfound freedom because I've always been very spontaneous. I've always been kind of an impulsive kid. And this was long before I started the dopamine agonist. So it has nothing to do with my medication. But I'm a little worried about what I'm going to do once, if and when the stimulation gets turned on and I start reaping all the benefits from this. Because 36:01Parkinson's has taken away my freedom. It's taken away my liberty. It's taken away my ability to do the things that I want to do with my day. If suddenly at the flick of a switch that gets restored, I have no idea how I'm going to react. I have no idea what I'm going to do. I hope to be as present in that moment as I possibly can be. But suffice it to say, it's something I'm deeply looking forward to. Sounds great.
Andreas Horn From the outside, we often see motor motor first, right? And that's the main thing we often see in That is maybe why Parkinson's disease has been classified as a motor disease. Would you think it was also to some degree liberating in terms of thoughts? So the inner world? Is that also was that also shackled by the disease? Or is that wrong? To assume?
Benjamin Stecher Yes, even in speaking with you now, I can't communicate as clearly, 37:01as I'd like to. I can't, because part of my attention is on my foot that has a tremor in it right now. Part of my attention is on my hands that can't move as fluidly as they used to. Part of constantly part of your cognition is taken up by this disease, whether it's in the background or not, whether it's whether you're focusing on a symptom or not, whether you're trying to mitigate something, you're always partially distracted by the disease itself, as long as you feel the imbalances and the lack of coordination. And the lack of fluid movements that this disease brings about. I look forward to not having to spending a day at some point in the near future, where I don't think about the word Parkinson's, or I don't think about this disease. I think that that's what I'm most looking forward to than anything else. Having my mind free of these symptoms that I experienced. I think that will be the greatest gift that I could possibly get. I just took a walk with Christos Ganos. He's also in Berlin. I don't know, you probably know him. 38:01As well. He's a movement disorders specialist at Charity. And I told him what what should I ask
Andreas Horn Ben Stecher? And he, he came up with the question. Do you think Parkinson's disease is a movement disorder?
Benjamin Stecher No, I would classify it as a communication disorder. Communication, obviously, between the cells and your brain. But more to the point, it's a break in the circuitry. It's dysfunction of those neural pathways, of those electrical currents that drive your ambitions, that drive your desires, that drive your motivation, that drive your hunger, that drive your feeling of satiation. To call it a movement disorder does not do justice to everything that it does and everything that it is. 39:01It puts it into a category. And it's in some ways is a helpful category. But it doesn't come close to describing the totality of what this disease is. So yes, Christos was bang on in his suspicion. I would not classify it as movement disorder. Going back to the surgery, a day after you tweeted that you experienced your first day in five years on which you did not experience an off phase. You already briefly touched on that. But can you maybe
Andreas Horn tell listeners? And more what that means?
Benjamin Stecher Sure. So, Parkinson's is often is for me anyways, the way I experienced Parkinson's is characterized by these fluctuating on off symptoms that I experienced throughout the day. I basically ride almost a sine wave of on off. So I take my first pill at about 738 in the morning. I turn on which is usually a dyskinetic time for me, I usually experience quite a bit of dyskinesia. That lasts for about an hour and a half to two hours. 40:01Then I slowly drift off where the medication stops working properly. And then I have to take it again to get back on. So that sine wave that fluctuating curve is the rhythm of Parkinson's disease for a lot of people, at least that's what it was for me. That day afterwards, that sine wave was flat. I had no fluctuations in my symptoms for that for that one day. That's coming back to what I said before, that ability to predict what's going to happen next. That ability, that freedom from that pattern of existence that I lived before and that I'm back in now. That was a joy to experience and a joy to go through. If I could, if I would do it all again, just to live that day. Wow, that sounds great. And maybe we should mention briefly that I guess your system, 41:01is currently switched off. So that is often referred to as the stun effect or honeymoon phase. So we can expect similar improvements later, but maybe not now. So it's normal. I just wanted to mention, it's normal that you're worse now. And I know you know that, but maybe the listeners don't. So I wanted to briefly mention it. Yeah. Yeah. And honeymoon is a good term for it, I think as well, because it does feel like you're free from everything that came before it.
Andreas Horn Super. Day two after surgery was worse. Can you explain why?
Benjamin Stecher Well, for one, I had the battery inserted and the wires tunneled through the back of me. That was much more painful to wake up to. It's a much more painful procedure. And it creates a lot more damage, I think along the way as well. Also, it's much more restricting in your movement. So for the, for at least the next three or four days after that second surgery, I couldn't move my right arm, or at least I couldn't move it without feeling that sharp 42:04pain in my chest. Anything and everything that made me stretch or pull on those muscles around my chest, anything and everything that had any effect on the muscles there was extremely painful. I felt those sharp tinges of pain immediately. Also, the wiring, it still bothers me to this day. It's actually probably my biggest complaint right now is you feel the tunneling, you feel the scar tissue forming, and you feel just a lack of flexibility in your neck. I think it Yeah, it's something I'm still grappling with. But it can feel it dissipating over time. It's getting easier and easier and easier every day.
Andreas Horn But yeah, that that second surgery is much more painful. And I'm hoping and from what I gather,
Benjamin Stecher this is the way we're heading, then we figure out a way to do this again, to do this kind of surgery 43:04without that second stage. I don't know if it means putting the battery in the cap of the
Andreas Horn electrode or whatever the technology might be needed to make that happen. But yeah, if the
Benjamin Stecher surgery was just the brain surgery, as weird as it might be to say, this would be so much simpler for the patient, so much easier on the patients. It's really good to know because you would think
Andreas Horn the opposite, right? And to ask again, it was not the second surgery itself, but waking up to it, right? Is that correct? So you were asleep for that one? Yeah, I was asleep for that one. Yeah,
Benjamin Stecher and it was the pain of the healing process that comes afterward. You participate in a trial of adaptive DBS and also wrote a blog post about that, what that means.
Andreas Horn Could you let us know? So there's not a whole lot I can say at the moment,
Benjamin Stecher simply because we haven't started the trial. There's still a lot of things that need to be 44:03worked out, so I can't get too into it. I mean, just the general concept of adaptive DBS.
Andreas Horn Yeah, so this goes back to my discussion with Hagai Bergman. That idea of closing the loop,
Benjamin Stecher that idea of having that feedback system in place so that not only are, is your brain responding to this new stimulation inside of it, but the stimulant itself is responding to what the brain is doing. That is a very attractive notion to me. I think that that is the key to really delivering personalized care for people with Parkinson's disease. Because throughout the day, everything changes constantly. If I'm running, if I'm eating, if I'm sleeping, if I'm sitting at a computer typing, I have different needs at any of those moments. And I need something that can adapt to each of those given times. I need something that can change over time, not only throughout the day as I experience different things, but as my disease 45:03progresses over time as well. I'm sure that more things will come up that I need to address. It's imperative that these devices are able to change over time. Even better if they're able to learn and adapt as the trial states, or as this new technology promises.
Andreas Horn Simply because, yeah, it has to be flexible enough to, life is not static. Life is not
Benjamin Stecher an end process of itself. Life is a continuum. And if you don't have something that can adapt on that continuum, that can ride those fluctuations with you, then it will inevitably become more and more obsolete the longer time goes on. I totally agree. And I mean, just as a general remark or background information for listeners,
Andreas Horn so the normal continuous DBS would just be on all the time, wouldn't respond at all to your brain, right? But what you're now trying, or the team is now trying in Toronto would be to sense
Benjamin Stecher 46:06at the same time, so sense the brain signals and then respond to that. So, of course, as you mentioned, this could mean that when you move, it stimulates differently than maybe when you don't move.
Andreas Horn Yes, exactly. Hopefully, it'll learn my patterns and learn,
Benjamin Stecher learn how to adapt to things over time. But also, I'm wondering, and this is, I have a question for you, if you don't mind. Sure, of course. How it works, how DBS works. Now, obviously, this is something that I don't think anybody
Andreas Horn can really pinpoint. No one knows exactly how it works. But the idea that the brain is going to be,
Benjamin Stecher so right now, I have these electrodes freshly implanted in my brain. And my brain is trying to figure out what to do with this new foreign thing. And I'm sure there's all sorts of glial cells that are responding and forming scar tissue. But once the device gets turned on and the stimulation starts, 47:02it's going to need to adapt to that new stimulant. However, if the stimulation itself is adapting, as the brain is adapting, closing that loop, closing that feedback mechanism, I'm assuming that they figured out how to do this, but I don't know how, I don't know for myself
Andreas Horn how that works. Do you think that's going to work? How that works? Do you have any insight that you might be able to share with me?
Benjamin Stecher It's happy to share everything I think, but it's so funny. I just want to mention that my next question would have been, how does it feel to undergo a procedure of which we cannot fully tell how it works, but only that it works, right? So I think in your book, you also said, quoted George Church, who's a geneticist at Harvard, who said, we developed effective smallpox prevention back when we had close to zero understanding of virology, and immunology. So essentially, I wanted to ask you the same question. My two cents on it 48:01would be a few things. So first of all, I think we can only, with DBS, we can only, you know, we cannot inject meaningful information currently to the brain. And with meaningful information, I mean, information that could substitute something that's not there anymore, that's physiological, you know, some complex as you say, communication in the brain, we cannot inject that. I mean, not yet. People are working on these things, but that's far ahead in the future. So what we can do, I believe, is rather to disrupt information flow. And of course, we don't want to disrupt the good information flow,
Andreas Horn but the pathological one, right? So the information flow that has gone haywire to some degree, and
Benjamin Stecher that might be one reason why, you know, both lesioning to the subthalamic nucleus and DBS
Andreas Horn 49:01works. Why also, it seems to work in, to be honest, in quite a few diseases, right? It does work in
Benjamin Stecher stonia, even the STN, it's not that popular, but it would work. And then in Tourette's disease, even an OCD, slightly different target. But it seems to me like there needs, first be a pathological signal somewhere that we could then modulate with DBS or tune down or tone
Andreas Horn down. And then maybe the physiological information is free to flow again, right? So maybe we reduce
Benjamin Stecher bandwidth, we shift, sorry, we reduce the pathological signal that is taking up all the bandwidth and that it makes it possible for the real information or the good information to flow again. And that would have to be a pathological signal. So I think that's a good idea. And then we have a few implications. For example, I would predict that if we would stick an electrode in my brain, not much would happen. And I would probably not develop dyskinesia, 50:06right? So again, I think something, so something would happen, of course, but, you know, not dyskinesia probably, because we would need the pathological signal first, which fortunately for me is not there. And, um, I guess the second part of your question would be with the adaptive DBS. And I guess this is a trial.
Andreas Horn I have no information, of course, of what is exactly is happening, but in the adaptive DBS
Benjamin Stecher trials that have been there so far, um, people have looked at the beta power often that that's one marker. And that is, you know, over 10 years described, a really beautiful marker that really codes, it seems, for symptoms of the disease. So I think that's a good idea. 51:23can turn on DBS and disrupt that pathological synchronized information flow. So that's my two cents. I must say, though, I'm in the imaging world in DBS, in Parkinson's, so I'm not an electrophysiologist. And this is just how I understand and treat the disease currently in my brain. So I think maybe just to finish this, the third part of your question was, you know, if that would now adapt to each other, that's a great question. You know, if you move, beta also goes down. So then how does the device know you move and so on? I think that's really ongoing 52:05science here, where people start using machine learning and so on to better decode what really is happening in the brain. So use a more complex marker than just beta power. And I assume you now have a device where you will always, you could always get the software upgrades to, let's say, implement the newest technology in this. So that could be great.
Andreas Horn Yeah. And coming back to your previous question about why I chose to do this,
Benjamin Stecher a small part of it was also just the opportunity to take part in this trial. I'm a natural born curious person. And the opportunity to play a role in helping us advance our understanding of ourselves and to understand our understanding of this disease was very attractive to me. I also kind of think somewhat egotistically that I think I'm a good person to test this on, 53:02not only because of my symptoms and my age, but because I have that curious nature in me. I'm going to be tweaking things regularly as we go. And yeah, I think it makes for interesting experiments. There's so many experiments I want to do. There's so many little things I want to try. After this gets turned on and after we start programming and fiddling with the devices, I'm excited just to be a living, breathing experiment onto the world. Yeah. And I guess you're right that from a scientific perspective, you are
Andreas Horn a perfect patient. That's true, right? You're young. You can maybe take part in experiments
Benjamin Stecher that take a bit longer and so on. And you're also very sharp and so on. So that is true. And in a similar, fashion it's really so special and unique to interview you um because of the many not only 54:01because you're young but also because of the many insights you have acquired over the years you know so you have so much interest in the disease and now you experience it so so that makes it such a unique and um yeah very um invaluable experience to interview you so i wanted to touch upon a few more smaller topics before um i let you go for now um your twitter bio reads consultant and advocate in biotech pharma and academia pushing for what is needed to properly treat and care for people with neurodegenerative diseases um you also work and i didn't identify as a patient advocate could you tell us more about
Andreas Horn that work and why you're doing it and what you're doing it for why it's important yeah so along the way i visited dozens if not over a hundred different
Benjamin Stecher centers, just trying to understand what the latest and greatest in this disease was, and I saw along the way that there's a dire need to bridge the gaps in these various communities because i was 55:06shocked how many times i was the first patient to ever walk into one of these centers and either give a talk or even just interact with some of the researchers there's so many scientists that have come across who who think that they are studying parkinson's or think that they're dealing with parkinson's when really they're just dealing with cell cultures or mice or and they have very few interactions with the human beings living with these diseases and i understand the need on some level to maintain a distance uh to not to so you can be a little bit more dispassionate about what you're researching so that uh you're not biased in any way as well but there is i mean it's a very human phenomenon. As far as we know, it only ever happens in the wild in humans. a lot about our behavior a lot about our social interactions go into this disease and if you don't take the time to try to understand these things if you don't take the time to try to understand 56:03what a patient is going through if uh i think you'll you're just missing so much of what this disease is you can't claim to know or be studying this disease even if you don't know what real human beings are experiencing and that it hits home every time i see mice every time i see
Andreas Horn mice in a lab you know 500 genetically engineered mice that live exactly the same lives they're raised in exactly the same environments they're bred in exactly the same way they eat the same
Benjamin Stecher food they do everything the same no two human beings even take identical twins uh will will be able to simulate that experiment if we were kind of reverse engineering this in some ways and going from the mice to the instead of trying to recreate what we see in humans and well that's actually a weird way of explaining it but anyways um it's important to know that animal models and the models that we have they 57:05can help us answer very very specific questions they're very they're great in helping us understand the fundamental biology they'll never be able to encapsulate the human experience and they'll never be able to tell you what parkinson's does to a person yeah i i totally agree with you yeah so um well maybe maybe toward that what will the future bring then then so three questions your future with dbs what's what what steps are next but then also maybe your personal future or the plans you have and goals you have in your life and then also the future of parkinson's disease research clinics big questions I've been told I need to be patient. That's probably going to take a while to get these parameters right it's probably going to take a while for me to find the right tuning 58:03but if i get to that point if i if i get to the stage where they turn it they flick a switch and i feel more like i'm not going to be able to do it i'm not going to be able to do it my future will be different than if I feel 50% back to normal, or if I feel 25% back to normal, or if I feel no benefit at all, each of those things will bring about a different future for me. So, 59:00and this is something I guess, I didn't fully appreciate before the surgery, although I knew it on kind of a philosophical level. I didn't appreciate how, how much of a fork in the road this is for your entire life. because depending on the outcome, you're able to do so much more. And that's like Parkinson's has taken away from me, my ability to be productive in the world, my ability to be completely independent in the world as well. I can't do all the things I want to do right now. If suddenly all those things are given back to me, I don't know what I'm going to do, but I, I, I hope to have this. I hope it's a problem I'm going to have. I hope it's something that I'm going to be facing. But I can't see past that moment at this point. I want to experience it. I want to live it. I want to be in that moment. I want to know and see what that feels like, but it's too hard for me to, there's too many variables at play for me to see past it. 01:00:00Now as for Parkinson's in general, and the future of Parkinson's disease research, I see it as, so I often stand back and look at the field, and I see it, this is going to sound derogatory, but it's not meant to be derogatory. I see it as almost like a hundred monkeys, sitting at a hundred typewriters trying to come up with Shakespeare. Each researcher, each scientist is kind of working on their own thing. There's domains and subdomains of this disease. There's the genetics field. There's the iPS cell culture field. There's so many different branches of research going on. Many of them are siloed. Many of them are not coordinating with one another. At this point, picking a winner, knowing who's going to emerge, knowing which branch of research is the most promising, knowing which studies are going to be the most promising. It's too hard to do. 01:01:01At the moment, I think we have 150 different molecules in clinical trial at various stages, either for symptomatic benefit or for disease modifying benefit. I look forward to seeing where this goes. Uh, I've become, I love to make predictions, but I, um, I'm also careful and wary of doing so, but I would say I can see the biases setting in now. I can see the biases creeping towards these electrical thinking of thinking of the brain more as a byproduct of the electrical inputs that it gets. And then these feedback loops that exist within it. I think biology is a great, subject to study. Chemistry is a great subject to study, but the physics of how the brain works, uh, might supersede all of those things. And it might be more, more paramount of all of the different branches that we're studying. 01:02:00I know that was a very meandering response to your question. I'm not sure if I actually know it was perfect.
Andreas Horn Yeah,
Benjamin Stecher no. And, um, and I agree there's so much, there's so much that can be done with, with things like DBS and thinking more about it. any monster in the room i don't know if you know that analogy but i know it yeah test of variants
Andreas Horn exactly um this won't be a cure but this will be this might be the best way possible
Benjamin Stecher to manage this going forward especially if the sorry if the technology continues to improve 01:03:00and we can get those electrodes to the point where they're razor thin and we don't have to have this battery and these wires implanted i imagine a future in which it's almost like a acupuncture therapy in some sense um another point i want to make something i'm realizing as we're talking is um my train of thought my ability to be lucid my ability to be verbose at this point has changed as well and i will i'll be very curious to see if we do this again at some point in the future how my responses to some of these questions changes over time because i i'm just noticing as we're talking that uh my train of thought is different from what it was prior to the surgery yes prior to the surgery and and do you what do you think in a good good sense or yeah in a very good sense um it's probably both in a result of the physical changes that i've undergone but also just the emotional changes the psychosocial changes um i think like i said before it's very much a fork in the road moment 01:04:06getting dbs and going through the trauma of the surgery as well and i don't think there's any way other than it changes you as an individual it changes in some sense who you are and what you are but see that's that's what i probably was referring to back before when i asked was it also liberating in terms of thoughts and i didn't really mean you know that you constantly have your symptoms in mind but rather that to me or to others as well, for example, Gyorgy Buzsaki has mentioned that for him a movement is a thought is a bit like a movement but it doesn't you know then go to your muscles so it would rather interact within the brain but you know to really have a thought to have a thought emerge that might be analogous to initiating movement without the motor output and and we are always so biased in a lot of diseases including also stroke 01:05:02with language and so on, where our Broca's area has a language error, you know, we see that first of course from outside you see movement and you see the movement and you see the movement and you don't see thoughts and of course we have all these instruments and so on but few people have the insight that you now have to really see them the internal world you know what changed in your brain beyond movement and i've noticed that the machinations and machinations is the wrong word but the way my thinking pattern has changed it's it feels suddenly different than it did before maybe i'm seeing something that's not there maybe this is um all in my head but i'm not sure i'm head as it were it is sure i feel like the same person i i feel like the same i have the same sense of self i obviously have all the same memories all the same things that were there before but there is like a subtle tweak of something that is there and i noticed this also the day after the surgery so i took part in an experiment on the wednesday thereof 01:06:02uh where they gave me a very very very minor stimulation and had me do a bunch of memory tests um
Andreas Horn That was an interesting experience as well, because you wouldn't think that the STN is so intricately involved in memory.
Benjamin Stecher But stimulating the STN, I think I didn't see the results of the experiment myself,
Andreas Horn but I feel like I did better on the memory tests when the stimulation was on versus when it was off. It does receive input from nearly the whole prefrontal cortex, right?
Benjamin Stecher So it is in its entirety, it is involved in a lot of things.
Andreas Horn Yeah, so interesting.
Benjamin Stecher We'll see, hopefully, if we can repeat this, how things progress.
Andreas Horn So that's really amazing. Maybe just to wrap up, is there anything else you wanted to cover that we haven't covered yet?
Benjamin Stecher I guess one part of it that I'm a little wary of is the stigma that will be associated with individuals afterwards. 01:07:05That's something I spoke to a little bit about with a friend of mine who had undergone DBS before. But there is a bit of a change in how you're perceived by the rest of the world as well.
Andreas Horn Interesting.
Benjamin Stecher And that, whether it be for better or worse, because especially for people for whom the brain is kind of a foreign substance, people who have no knowledge of neuroscience, people who have no understanding of what the brain is doing and how the brain thinks and how the brain works. I think to them, this is a, not only is it a very scary thing, obviously, but it's very, alien, it's very foreign. It's something that they have no connection to. It's something that they can't internalize in any way.
Andreas Horn They can't, yeah, there's just no reference points for what I've been through.
Benjamin Stecher I've noticed, I think, and this is maybe, again, me looking too much into these things, 01:08:01but there is a slight change in the way the rest of the world perceives you.
Andreas Horn It'll be interesting to see over time how, to take note of that and to see, I guess,
Benjamin Stecher continue to follow up on that line of thought.
Andreas Horn And you mean your direct, like, friend, friendship circle around you, people around you, or do you also think now in your special case, since it's a bit more public, also the public appearance of both of it? Yeah, all of it.
Benjamin Stecher There's no one that I interact with other than like maybe my nephew and niece who are a little too young to understand anything at this point. There's no one who, every relationship changes, I feel like. Every connection I have to every other person is a little bit different than it was before. To my parents, to my friends, it's not necessarily good or bad. It's not necessarily, you know, moving away or moving towards. 01:09:01It's just different. It's altered. It's an altered state, I would say. I mean, it could be that it's also just new to most and then. Once they find out you're the same Ben, you know, things get to normal. So that could also happen. It could be. That's true. And I'm sure it'll change over time as the stimulation starts and as the therapy hopefully sets in.
Andreas Horn Yeah. Yeah.
Benjamin Stecher Great, Ben.
Andreas Horn So thank you so much once more for participating.
Benjamin Stecher This was really unique and very helpful, insightful for me. And I'm also sure to all the listeners. Thank you. Actually, sorry, there is one other thing I wanted to say. And that's. Sure, of course. To the patient community as well, especially to patients who. So I have a lot of patients now reaching out to me, asking me how I'm doing, how it was. Some of them are preparing to go through this themselves. I can't. I know everyone kind of wants somebody to make some of these big decisions for them, I think. 01:10:03Or they. They have it. It's a very difficult thing to ask anybody to do for themselves. But you have to, on some level, try to understand what you're going through. And I've noticed in the materials I've gotten since that there is no patient guide to DBS. There's no good patient guide to DBS. There's no manual that tells you what you're going to go through. That's a good point.
Andreas Horn Yeah.
Benjamin Stecher Everything is novel. Everything is kind of new along the way. And you have to be ready for that. You have to be ready for all the ups and all the downs.
Andreas Horn Yeah.
Benjamin Stecher And again. I guess one last thought. I haven't been able to articulate myself as well as I would like during this interview. Not that I'm in any way unhappy with what I've said. But I'll be interested to see, I guess, how I might respond to some of these questions a little bit differently in the future. I would love to repeat it if you can find the time. 01:11:00As we discussed before. So that would be great.
Andreas Horn Okay.
Benjamin Stecher Awesome. Super. !
Click any highlighted text passage to jump the Spotify player to that point. The transcript text is present directly in the page HTML for search engines and accessibility.
References relevant to the episode
- Ben’s blog, Tomorrow Edition
- Pre- and post-operative video interviews of Ben on his youtube channel
- A link to the book Brain Fables, authored by Alberto Espay and Benjamin Stecher
- Ben on twitter
Colleagues mentioned in the episode include
- Alberto Espay (Neurologist in Cincinnati)
- Hagai Bergman (Neuroscientist & Neuroelectrophysiologist in Jerusalem)
- Alfonso Fasano (Neurologist in Toronto)
- John Hardy (Geneticist in London)
- Anatol Kreitzer (Neuroscientist at UCSF)
- Bas Bloem (Neurologist in Nijmegen)
- Anthony Lang (Neurologist in Toronto)
- Eric Kandel (Neuroscientist in Maryland)
- Christof Koch (Neuroscientist in Seattle)