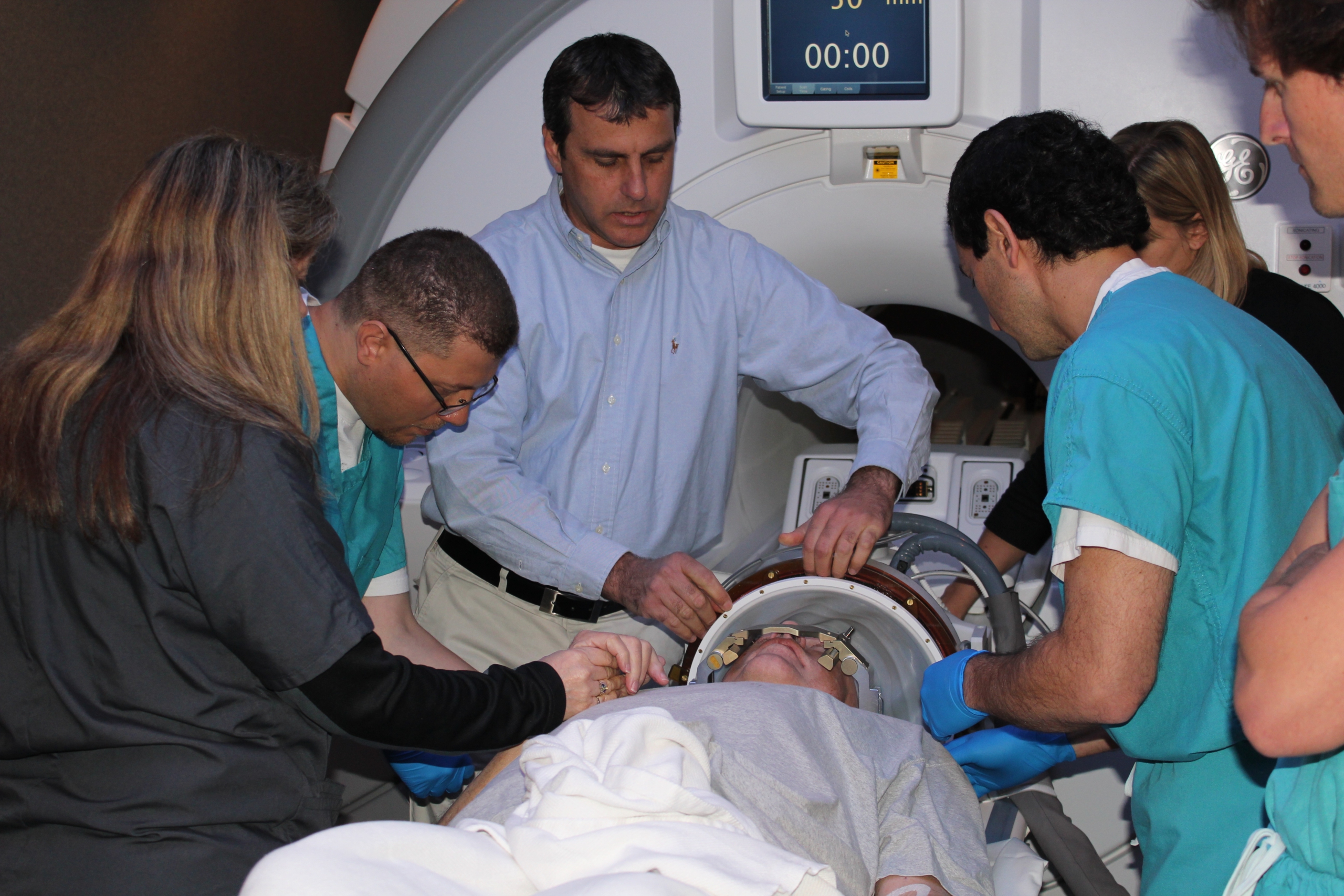
Dr. Eyal Zadicario is the COO of Insightec.
#73: Eyal Zadicario – Beyond the Scalpel: Towards an Acoustic Neurosurgical Suite with Insightec
In this episode of Stimulating Brains, we sit down with Dr. Eyal Zadicario, Chief Operating Officer at Insightec, to explore the remarkable evolution of focused ultrasound – from its experimental origins to its transformative role in functional neurosurgery today.
Dr. Zadicario shares insights from over two decades at the forefront of innovation, reflecting on the challenges of translating breakthroughs from academia to industry, designing clinician-friendly systems that prioritize the patient experience, and overcoming skepticism toward disruptive technologies.
Together, we revisit key milestones – from the first MRgFUS based thalamotomy in 2008 and early applications in breast cancer, to the expanding frontiers of neuromodulation. Looking ahead, we discuss the exciting possibilities of blood brain barrier opening, the acoustic neurosurgical suite, and even brain mapping through focused sound.
Tune in for a fascinating conversation on how precision acoustics are reshaping the landscape of brain therapy and beyond.
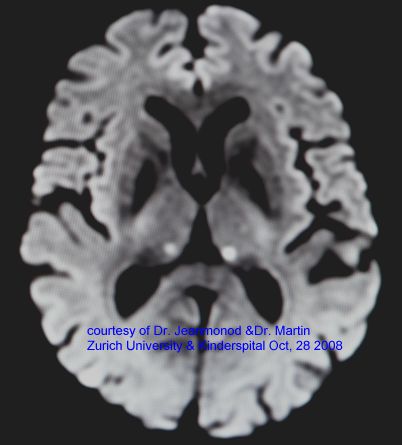
Eyal Zadicario 00:00By the way, neuromodulation from the way we saw it back then was the most challenging because the accuracy, the precision, the side effects in the thalamus, as you know very well, it's very, very demanding. September 23rd, 2008, it's a time to remember where the first non-invasive thalamotomy was done in a neuropathic pain patient. And we kind of felt this was maybe the biggest eureka moment of saying, hey, now we got it right. And our ultimate goal is that the patient experience will be such that every patient that can benefit from a treatment will actually get it. So I think at whole, our vision would be that in neurosurgery, there would be an acoustic neurosurgery platform that can actually treat any surgical target, not invasively. That's our stuff. No radiation, no incisions. And there will be a day when we will see. Why did we cut the body to destroy that target? 01:00There are non-invasive ways to destroy that target that are safe and effective.
Andreas Horn Welcome to Stimulating Brains. Hello, and welcome to Stimulating Brains. In this episode, we sit down with Eyal Zadikario, who's the chief operating officer of Insightech. We trace together the history of focused ultrasound, from its early experiments to its groundbreaking role in functional neurosurgery today. Eyal reflects on the challenges of translating innovation from academia into industry, and And he's going to talk about the challenges of translating innovation from academia into industry, designing clinician-friendly interfaces that truly focus on the patient experience, 02:05and working through the skepticism that comes with any disruptive technology. We dive into various pivotal milestones, like the first non-invasive thalamotomy, which happened back in 2008. We also talk about the early beginnings of focused ultrasound in breast cancer, and then how it evolved. And then we talk about the early beginnings of focused ultrasound in breast cancer, and how it evolved. We tackle an even more challenging task in neuromodulation. Finally, we take a look at the future. We discuss things like opening the blood-brain barrier, the vision for an acoustic neurosurgical suite, and even brain mapping with such technology. I hope that you enjoyed this episode as much as I did, and thank you for tuning in to Stimulating Brains. We'll see you next time. 03:26Bye.
Eyal Zadicario Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. 04:00Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye. Bye.
Andreas Horn Fantastic. And I see the ocean behind you, right? The sea. Is that something you enjoy too?
Eyal Zadicario Yeah. So, you know, our offices in Israel and Haifa are right on the border of the Mediterranean, which is what you see. It's a great view, but it's a great joy to come to work every day, driving along the coast here in Israel. I drive all the way from Tel Aviv to Haifa every day.
Andreas Horn So it's a nice one hour drive along the coast. Oh, okay. Fantastic. All right. So can you talk a bit about the vision and also how InsightTech was founded? So how it all started? So InsightTech was founded with the vision to
Eyal Zadicario improve patient care. I mean, you always start and look at the patient first, not so much with the technology. So we looked at surgery. And when you think about the holistic approach of surgery, which has been practiced for decades or centuries, the tools have advanced, but the concepts stay the same. You have a target pathology, you need to usually, 05:03physically get to it, identify it, feel it, visualize it, and then either treat it, remove it, or do something physically in the body. And our intent was to find a technology or a treatment modality that can do that with not impacting the surrounding tissue. So no incisions and no harm to anything but the pathology that you wanted to treat. And that's what the concept that drove us to look into ultrasound and focus ultrasound. The treatment modality that can actually do that, that can target a pathology impacting and affecting only that pathology and leaving the entire surrounding area, the skin, the bone, the tissues around the target area, completely unaffected or intact. And that was the vision
Andreas Horn that we started with. Why ultrasound? Why not? You mentioned radiation or other options. Why 06:02ultrasound?
Eyal Zadicario So ultrasound has a very unique capability. It can penetrate the body. And we use that for diagnostics and for imaging. So it can penetrate both superficial parts of the body and deep in the body. It's really, really effective in penetrating the body. And in certain doses,
Andreas Horn in certain parameters, it has no impact, which is why we like to use it for diagnostics.
Eyal Zadicario And on the other hand, it has no accumulated effect. You can pretty much repeat with ultrasound as much as you can, unlike radiation. So there's no dose limit to how much ultrasound you can apply without creating damage. So that's another great attribute of ultrasound. But the main thing is that ultrasound can be focused. It can be focused like a magnifying glass focuses the sunlight to create a very high intensity area 07:01in the body with a lot of energy. Or very high intensity energy, while the other surrounding volume around that target or around that tissue has no, no, as an energy that's low enough to have no impact on the tissue. So it can be highly focused. The fact it can penetrate the body and the fact it can be highly focused are the two attributes that ultrasound has that no other treatment modality has.
Andreas Horn It's really, really interesting how much, you know, ultrasound, like the potential of it, right? We, we, we currently at a, at a state where with the insight tech device, for example,
Eyal Zadicario lesions are being burned, but of course there's also the blood brain barrier opening. There's potentially even functional like diagnostics of ultrasound. We, we, we can maybe get to that bit later, but, but I agree with you. It, it has like, as a general premise, it really has many properties that are on the wishlist of what we want to do in the brain. So 08:02focused ultrasound,
Andreas Horn was there before what was different or how, how did the company found like how, what was different when you guys started off or what is different in the approach?
Eyal Zadicario Yeah. So, so when we started, as you, cause you mentioned ultra focused ultrasound and not to mention diagnostic ultrasound, but also focused ultrasound was there for decades before we started. And the fact that I just mentioned around ultrasound being that you can focus ultrasound, that you can, that you can, that you can, that you can, that you can, that you can, that you can, you can penetrate the body, that it can even be used for lesioning or, or ablation was, was known before it's like the camera. I think our biggest contribution and, and, and, and now they advanced was the fact that we've learned that with ultrasound, the variability of how tissue and ultrasound, how the variability of how ultrasound interacts with tissue or the interface between the tissue and ultrasound have a lot of variability. They depend on the vascularity, 09:02the type of the tissue on the pathway to the target. And really all the uses of focus ultrasound in the earlier decades by great pioneers showed that it can be done, but were not able to, I would say, make it a predictable and robust medical device. What we added was the closed-loop aspect. The fact that, like in surgery, I mean, you can plan the surgery. At the end of the day, when you cut into the tissue, when you get to the target, you actually need to visualize what's happening at the target point and adapt your treatment parameters or your treatment plan to the actual anatomy and the actual response of the tissue to the treatment. We call it closed-loop in a technical term. And this closed-loop allows us to not only visualize the target we are aiming to treat, but also get some feedback in real time. 10:00And there's different feedbacks for different modes of action. But the ability to get feedback on, for example, thermometry from the target when we're doing thermal ablation is a key aspect that actually transforms focus ultrasound from just a potential therapy to a very precise lesioning technology. And without that closed-loop, without making sure or confirming that you are actually on the right target, without actually modifying in real time the parameters to get the temperature that you want, this would never become a precise and predictable medical device or therapeutic tool.
Andreas Horn Okay.
Eyal Zadicario So the measure that you can measure, for example, the heating with the MRI in a closed loop and then while planning kind of increase dosage, that's the key contribution or the key difference that made it a real therapy.
Andreas Horn Very interesting.
Eyal Zadicario I have talked to collaborators. 11:00I have talked to collaborators. I have talked to collaborators. I have talked to collaborators. I have talked to anthropologist ! Yeah!
Andreas Horn But the MR guidance, is that another key point that was important to overcome the hurdle of the skull? Yeah, so actually, the ultrasound in general does not penetrate bone very, very well.
Eyal Zadicario Or actually, very little of the ultrasound energy penetrates bone.
Andreas Horn That's why you don't hear about ultrasound being used for brain diagnostics.
Eyal Zadicario You use either MRI or CT or other diagnostic modalities because most of the ultrasound does not penetrate through the bone. And actually, we did not start as a company with the brain right away. We originally worked on breast cancer.
Andreas Horn 12:03Okay.
Eyal Zadicario Because maybe from a technical perspective, the most obvious choice to start, because it's a well-identified target, can be very well visualized on MRI.
Andreas Horn Okay.
Eyal Zadicario You can actually, it's almost external to the body in a sense that you can target it without going through a lot of abdominal or other structures to get to the target. So that's where we started. We thought that the brain was too challenging because the skull is just not penetratable for ultrasound. And we started with breast tumors, which we've learned a lot. And basically, what I mentioned earlier, the fact that although you can target the ultrasound, you can target the ultrasound at the right point, you still need that feedback because different, even in the breast tumors, different tumors have different attributes and different parameters needed to actually get to the right temperature and treat them, was a lesson learned back in those days. 13:00The tissue variability is a key thing. And if you don't account for that, if you don't adapt your therapy based on the actual response of the tissue to the ultrasound, then you're never going to be able to do. So we started with breast and then moved on to other body parts like uterine fibroids, which was basically our first commercial platform. Again, this was a benign tumor in the uterus with a product that we put out back in 2004
Andreas Horn and got it all the way to commercial approval in 2004. Is that still? Is that still an active therapy, the breast tumors?
Eyal Zadicario It's an active therapy in some parts of the world still, but we have stopped commercializing that a few years ago. This was one of the, you know, there's something we can talk about later, but there's, 14:01I would say that the journey of focused ultrasound, with Instatec in general, has gone through multiple, you know, applications being developed. We know today that the brain is the one that commercialized most successfully for various reasons that we can discuss later. But we've learned a lot from the earlier experience with breast and uterine fibroids on how to really plan ultrasound, how to plan therapies to actually be very precise and predictable. And all these lessons learned on how to target, not to accommodate tissue variability, really came from the earlier, earlier, I would say experience with non-physiologic, not just the ! Dr. Dr. Dr. Dr. Dr. Dr. Dr. Dr. Dr. Dr. Dr. Dr. Dr. Dr. Dr. Dr. Dr. not transcranial, but actually soft tissue, soft tissue targeted soft tissue tumors. So to go back to your question about transcranial, this was when we started was kind of seemed impossible. People said that people were very skeptic that you can get ultrasound energy through the bone and keep it focused and get enough energy into the brain that you can actually 15:06treat without damaging the skull, without causing skull heating and skin burns. And this did require a lot of development, I would say initially on the focus part, because the most, I would say the biggest impact that the bone has on the ultrasound beam is that the variability of the bone, the non-homogeneous bone structure really disrupts a focused beam. So it's much more difficult to keep the beam focused through the skull with respect to any other soft tissue target in the body. So we basically in the early years of instead of establishing 99, we started working on the brain as a full program in the early 2000, like right when the company started and developing the transcranial focusing was the key, 16:02the key part of that, because without that, you could just could not get the energy to the right target. Now, even at that point in time, there were a lot of, there were a few academic teams working on that solution on how you can focus ultrasound through the skull. And there were, I would say simulation models that showed that this can theoretically work. Some experience in preclinical settings that on cadaver skulls and all kinds of models that show the potential, but here there's another element that I think is really important. And that's, I think, you know, I think that for a company is a little bit different than the academic challenges that solving the problem in academic setting is the foundation of how you innovate and you solve problems, scientific problems, but then developing that to a real robust medical device is a different challenge. That's where companies face a challenge that's a little bit different than academia, because you can have a great simulation 17:03for how the, to overcome the defocusing effect of ultrasound. The skull. But if that simulation is like takes hours or days to run at the time, like 20 years ago, then, then it's not useful in the clinical settings because every time you move the target, you have to rerun that. So a lot of the challenges of, I would say the real world challenges from a device perspective, from a, from a, from an industry perspective are different than just solving the academic problems. So that's where we focus our initiative and we really accelerate it. And, and innovated around how you can make a quick and real-time algorithms to actually focus through the skull and, and, and make sure that you're aiming the ultrasound at the right target. Yeah. I think in the beginning, you also collaborated or merged with General Electrics.
Andreas Horn Can you talk a little bit about that GE?
Eyal Zadicario Yeah. So when InsightTech was founded in 1999, it was basically merged its efforts in developing 18:04focused ultrasound as a therapy. with GE. GE had an innovation lab in the research center in New York that worked on focused ultrasound. Naturally, the first prototypes of the breast cancer study that we did from a systems perspective emerged between Insightec's technology and GE's technology. GE had a small research team working on ultrasound for breast cancer. And we merged those efforts when Insightec was founded. we basically took over the ge effort for therapy g wanted to focus on diagnostics with ultrasound and with all other modalities and insetec took that that program and integrated it into what has now become inside
Andreas Horn cool what was your first fda approved indication
Eyal Zadicario 19:00so the first fda indication that we we took to market was the uterine fibroids we basically in 2004 got that approved and we started working on that product in in 2000. so in four years we developed the technology and installed about 10 or 15 sites in the us and then ran a full clinical trial and got approved in 2004. and this was a treatment where benign tumors in the uterus which cause a lot of pain and bleeding discomfort and sometimes fertility problems for women need to be treated mostly the standard of care for that was hysterectomy and still is history and we offered to replace that with a two-hour procedure not invasive back home the same day by thermally ablating those tumors not invasively 20:00but ! ! with urine fibers. And some sites are still treating that, mostly in China. And basically from 2004 all the way to probably until six, seven years ago, this was our biggest commercial product for reasons that are more, not so much technically, but more on the market creation phase. We at some point in time decided to put our focus on neuro and focus the company around our neuro commercial efforts. 21:03And again, it goes back a little bit to what I said with compared to academia. And that's another lesson learned for many, you know, entrepreneurs out there. To succeed in the market takes much more than just a good technical solution. There's competitive landscape. There's economics around that. There's the biggest change in market, the biggest, I would say, challenging market creation that we are facing with bringing a new modality. That usually requires a pretty significant change in the workflow and the referral pathway of patients. Because we're bringing in something so new that it disrupts the current setting in the hospital and how therapy is being delivered. So that challenge is something that with urine fibers, we were successful in the technical part, successful in the clinical part, but at some point in time, focused our resources on neuro. And did not kind of bridge the gap 22:02to actually make it a big enough commercial success to focus the company on that. And we had to pivot and choose. And we pivoted and that's it.
Andreas Horn Interesting.
Eyal Zadicario But my understanding is that the uterine fibroid application also matured your understanding of, you know, like it probably paved the way to neuro.
Andreas Horn Is that correct?
Eyal Zadicario It paved the way in many ways. It paved the way because that's where we learned, you know, that there's more to treating with focused ultrasound than just aiming at the right target and turning the power on. There are structures you have to be careful with. There's just the skin that you have to wash so the energy is not too high on the skin to cause skin burns. There's bones behind the tumors that get some of the far field effect of ultrasound. Ultrasound doesn't stop at the target. It keeps propagating into that, into the bone in the far field. And dealing with that and doing all the treatment planning aspects 23:05of how tissue responds to ultrasound, that's what we learned the most. Because we treated thousands and thousands of patients of uterine fibroids. And we learned a lot about our thermal simulations, our acoustic simulations in real world tissue, where you have a lot of layers and fat and vascular chairs and all kinds of bone and learning how to deal with the heterogeneity of the tissue. And we learned a lot from that. And we also learned a lot on the, I would say, market creation efforts, how to impact referral pathway, how you can really, the importance of workflow, for example, in a medical device is just, you can't overemphasize that. I mean, you can have a great technology, but if the workflow, the clinical workflow is not smooth enough, routine enough, fast enough, easy enough, then you just run into a lot of hurdles. That's it. That prohibit the rate of adoption. 24:02And that's where we've learned that from the very, very former. So, so happy to talk a bit more about that. Right. So my understanding of what you've said was that you have a great technology that in theory works really well, but maybe it takes a lot of time for the patients to be in the right position, or even the billing is complicated or the device is complicated or these things. And then it just doesn't scale enough. Right.
Andreas Horn Is that what you're saying?
Eyal Zadicario Like, because then maybe you get it installed in one hospital. And they have some good experience with it, but moving it to the next one or doing high volume is really tough.
Andreas Horn Does that go in the right direction?
Eyal Zadicario There are challenges and you can kind of, you have to kind of go through all of them. I mean, you have to have a technology that works. You have to prove that it's safe and effective. You have to get, after you do that, you have to get the clinician, the patient, the treating physicians to really adapt and accept the fact that this is a meaningful clinical tool that they would like to use. 25:05Then you have to get it through regulatory. And once you get all through all that, then you start the market creation phase, which basically is really to your point, how you scale has a lot to do with the, or the adoption rate of how quickly you scale has to do with the referral pathway, the workflow, the competitive landscape, not just with other in my gutter focused ultrasound technologies, but other, you know, I'm not going to go into too much detail on that. I think that's a really good point. I think that's a really good point. I think that's a really good point. I think that's a really good point. I think that's a really good point. I think that's a really good point. ways to perform that procedure. We can talk about that in neuromodulation as well because there are other ways to treat, for example, tremor and Parkinson's disease, which is what we treat today. So your competitive landscape is not only your colleagues making the same technology. It's actually what other alternatives does the patient have to choose from. So I would say we've learned a lot in how to impact growth and scale 26:03beyond just developing the technology. Before pivoting to neural, you also had two other indications approved.
Andreas Horn What were those and what did you learn there?
Eyal Zadicario The second indication we got approved after intrafibroids was pain palliation for bone myths. Basically what happens when you have a primary tumor that metastasizes, metastasizes to the bone, that tumor at the bone both destroys the bone and is very, very painful. And we use the same body platform to treat and heat that tumor to a point where the nerve endings near the tumor were ablated and therefore relieving the patient from pain immediately. So patients that were suffering from pain which originated from bone myths could get pain palliation. And we get pain relief almost instantaneously after treatment, immediately after the treatment, which was no other therapy could provide them with that 27:01because there are alternative were either medication or opiates or radiation, which takes many, many weeks to really have an impact. So we got that approved. And I think that FDA approved. And basically that was another application to our body system which treated neural fibroids at the time. And the second one was prostate. We developed a transreptile approach to thermally lesion or ablate prostate tissue. Basically, instead of removing or doing a prostatectomy or doing a pretty radical surgery for prostate tumors, provided a focal therapy where you could actually treat only the tumor. You didn't need to heat or ablate the entire prostate. And that led to a much, much better adverse event profile or much, much less adverse events in prostate treatment for prostate cancer. 28:03So both of these got approved and went into a certain commercial phase before we pivoted and focused on the underlying. Like before we focus on neuro in the remainder of the conversation,
Andreas Horn do you think you might ever go back to these applications now that you're a bigger company and you know, could that happen?
Eyal Zadicario I think focus. Super sound has a lot of potential in body tumors and basically process specifically any other indication fibroids liver or others that we can talk to. I think that, that the fact that there's room for focus, super sounding many, many surgical therapies, I think is well established and understood that there's a lot of opportunities for us within the brain, but eventually now, you know, technically there's a lot of know-how. That's very, very relevant to other body parts as well. So there are potential in the future.
Andreas Horn Yes. Is it in our plans currently?
Eyal Zadicario 29:00No. But, but there's,
Andreas Horn there's a lot out there to do with what was for some of the body.
Eyal Zadicario Great. And so the pivot to neuro, like it, you know, it seems a bit like you, you were very successful, but there was, it was a bit hard to create a good market that was maybe sustainable for the company. Now pivoting to neuro seems almost in hindsight, like a more complicated, like finding an even harder struggle,
Andreas Horn right? So hadn't been done before was certainly not an obvious success. So how did that come? Was it, did you really see market analysis wise?
Eyal Zadicario This would be, if it works real niche where we can, you know,
Andreas Horn scale up or how was it motivated? How, how did you start and how, how did you then also address the challenges of the skull?
Eyal Zadicario So, so from a market potential and, and, and, and the technical challenges, these are two separate aspects. So I'll touch upon both. I think that first of all, 30:00we, we started the work on the brain actually in parallel to everything that we just discussed, just that it took it more time because of the techno clinical challenges to be ready for, for, for clinical treatment and then for, for commercial work. But we started that in part for both, for two reasons. One, we, when there, there's a huge unmet need in non-invasive brain surgery, which we can talk about in a second. And also we knew that if, if, if we could prove that focus ultrasound is safe and effective enough to treat the brain, not invasively, it would be pretty obvious that it could be treated. It could be effective in treating many, many other things. As you kind of mentioned, it's probably the highest barrier in terms of the technical clinical challenge. And the, the, the importance of, of, of accuracy, the not impacting surrounding tissues is probably the biggest challenges in 31:02the brain. But we felt that if we prove and we, we prove that that works, then that would open up a lot of other opportunities for us and for the field in general. And I think that, that realistically, I think it happened really happened. And, and the intent was to really touch that Holy grail, and make sure that if we can get that right, then then focus on sound has many other potential indications to follow. Great. What, what were key challenges and how you know, I know simulations were very important. You have to kind of simulate how the bone refracts the, the, the sound you had mentioned already before that just moving the spot a little bit would in the old days take, you know, 20 hours to calculate, calculate the new spot or something,
Andreas Horn right? So how did you overcome these challenges? So what were the challenges?
Eyal Zadicario Maybe talk a bit about if you could about the, 32:00you know, essentially setting us back into time. We're now in the year 2000.
Andreas Horn What, what did you guys do and what were the problems you had?
Eyal Zadicario Right. So I think, I think two, there, there's two elements that made that were focused on first one is the, the acoustic face of it, because, the face of the red is this, this transducer, this helmet by which you need to transmit energy into the brain is very, very different than the other body part for, for multiple reasons. One you touched upon is the fact that the skull is very non-homogeneous and has various thickness shape and, and, and various intensities or dense bone densities over, over different areas of the skull. And that requires a very sophisticated technology to shape your acoustic beam to go through the skull. 33:00We call it the focusing algorithms, but, but to, to implement that you, the face, the race system with hundreds or thousands of elements that can actually shape the beam to go through the skull. So there was the simulation part, but it was also the design and construction of acoustical phase, the race with thousands of elements that can, that can generate the beam to, I mean, it's one thing to program the beam and do the simulations. And it takes another piece of hardware, a lot of innovation development. How do you build phase the race that can actually have thousands of elements and can, uh, generate these beams to propagate to a skull. Now, keep in mind that we already knew that feedback is very important and we knew that we would need AMR feedback, but we also need to have feedback to measure temperature in the skull, in the brain in real time. Because again, it's a very unique, uh, 34:00uh, uh, aspect of what we had to develop because only MRI can noninvasively measure in real time, temperature in, in, in the body without having any probe or, or, or anything go in the body. And, and in the sense in the sensitive and, and, and real time enough way, to be, you know, one degree accurate and, and, and every three or four seconds get, get an actual temperature thermal measurement. So integrating the hardware into the MRI was another big technological challenge because you take two very complex systems, the ultrasound thousands element, phased array, the MRI, and have to merge these two together into one, you know, medical device, which is, it's really complex. So, it was sort of like 35:21And that was a big challenge at the time because you take all these complexities, you know, of the physics behind programming the array, the physics behind how to get thermal measurements in the MRI, binding and timing these two together and run all these complex simulations. But our concept from day one was that there needs to be a clinical decision making in real time. And therefore, the treating physician has to be able to operate his surgical tool. The fact the surgical tool is complex is kind of needs to be simplified to a way that a clinician can operate this sophisticated technology. So the user interface was a big challenge back then.
Andreas Horn 36:08How do you... How do you take all these complexities and make them into a workflow and control mechanisms and data visualization that the clinician can effectively understand, impact and control?
Eyal Zadicario And that, by the way, is still the more we realize how important that is, the more we invest and improve on that. And it's continuous improvement. I mean, the user interface we had back then is nowhere close to what we have now. Today, we use machine learning algorithms and AI to help us optimize and learn from the treatments that we do into improving algorithms all the time. But I started as a user interface back in 1999, where user interface was very different than what it is today. And then it evolved over the years. But I would say it taught me that the importance of simplifying. 37:06No matter how... No matter the complexity of the problem, simplifying it to the user, just like, you know, that it speaks in the language that the clinician understands and that it visualizes complex phenomena in a clinically meaningful way is the key to successful workflow and successful treatment at the end of the day.
Andreas Horn Yeah. And you have to make tough choices, right? We create an academic toolbox, Lead DBS, and there it's a bit different where we... Yeah.
Eyal Zadicario We have...
Andreas Horn We maybe want to even have more choices because it's still not figured out what the real workflow is, right? But even there, I mean, getting rid of buttons is not easy because you know all about it. You want both options, right? But then you realize maybe it's just overwhelming for users to pick them. 38:02So I can only imagine for a commercial product that you have to pick one, right? If there's two or three ways to do this... Yeah.
Eyal Zadicario ...you should make the choice for the user and then... All right. Can I...
Andreas Horn Yeah.
Eyal Zadicario Sorry. I'm just... Come back on that. I just mentioned how we did...So, so the system engineering teams have this saying that your design is perfect not when you have nothing to add, when you have nothing you can take away.
Andreas Horn Yeah.
Eyal Zadicario Because the idea is usually you start with a lot of features. And we started this in a research setting, which is one, I would say, typical set of cohort of clinicians.
Andreas Horn Yeah.
Eyal Zadicario And, and users. But today when we're working within a commercial setting or in a high scale commercial setting, the, the, the, what you talked about is actually very, very true because different users want different workflows and we have to sort of adapt between, on one hand, keeping the flexibility...
Andreas Horn Yeah.
Eyal Zadicario ...for each user to adapt what they like and how they like to use the system, but then have a very simple workflow that whoever wants a very simple workflow can still have that.
Andreas Horn 39:06Yeah.
Eyal Zadicario And we, we, we try to leverage, you know, balance that.
Andreas Horn Yeah.
Eyal Zadicario There's always a, there's always a lot of trade-offs there. Of course.
Andreas Horn Yeah. Can I ask when you entered, so you entered the company when it was founded, 1999 and... Yeah, the year it was, the year it was founded, yeah. How many people were working at Insight Tech at the time?
Eyal Zadicario When I joined Insight Tech, probably about 30 people or...
Andreas Horn Okay.
Eyal Zadicario ...between 20 and 30. This was early 95. So I joined in mid-99. The company was formally established in early 99. And so it was the first few months the company started.
Andreas Horn Yeah.
Eyal Zadicario Now it's a... It's a very different ship, I'm sure.
Andreas Horn Yeah.
Eyal Zadicario Oh, okay. At least it is.
Andreas Horn Okay. So with this, with these developments, we heard about the theoretical, you know, phase array beams, getting, like the simulations and so on. Were you ready to treat patients at the time?
Eyal Zadicario So, you know, our first neuroclinical prototype was ready in 2005, like probably five, six years after we started. 40:04It was the first ever transcranial clinical prototype. I mean, as you know, certain labs had various prototypes in preclinical testing. But we got to a point in mid-2005 or early 2005 where we had a clinical prototype that was ready to treat patients. And it had basically a similar helmet from the way you know it today, but very different from the design perspective. And we'll touch upon the progress made maybe a little bit later. But... In early 2005, we were ready to treat patients. It was one prototype that we built. It worked with the Brigham at the time and with Kulervo and then his lab and Nathan McNall in the lab. And basically we're ready for our first clinical trial. And we started with GBM because we thought that it was the right thing to follow and just treat tumors. 41:01Glioblastoma, right, for the naive... Glioblastoma, yeah. Glioblastomas. And... And we treated three patients between the first... In the first half of 2005. And this was definitely, you know, just a breakthrough from the fact that we... This was the first time ever that focused ultrasound was used in... Transcranially to treat patients. And definitely one of those eureka moments where you actually put ultrasound through the bone, in the brain, and a lot of, you know... There were a lot of skeptics that this... What risks and what other impact that would have on patients because technically there was no... Never before was there ultrasound placed at these intensities in the brain through an intact skull... Of course. Ever.
Andreas Horn And that was... 42:00And you could see it, right?
Eyal Zadicario You could run another MRI and see it. That's fascinating. So what we were able to establish...
Andreas Horn Yeah.
Eyal Zadicario We could see the MRI thermometry worked. We could see to a certain extent that the whole outlet concept of the workflow, the fusion between CT and MR and how we register all those and how we correct for the focusing has the potential to work. And we could actually establish to see a thermal spot in these lesions. But I must say early with that prototype, we also realized that we're very far from a real product. We learned a lot from these three patients. And we learned many, many things on the technical and the clinical aspects of that. First of all, this was not the same device we have today. This was a much less powerful system. It had only 500 elements compared to the thousand more that we have today. 43:03And it was just did not have neither the power nor the element. And. I would say accuracy to generate a beam that's powerful enough and focused enough. We also know early on we wanted to really, really stay non-invasive. So we used thermoplastic masks like using radiation to immobilize the patient during the treatment, which we thought from an engineering perspective that this would be ideal because we did not want to even use pins at the time. But it turned out that the patient moved a lot during the treatment. The treatment moved too much. It was really not tolerable and actually pretty painful for them. So after these three patients, we went back to the stereotactic frame. And I would say listen to a lot of neurosurgeons that just said, look, you got to keep the patient. And the easiest and most convenient for the patient to be immobilized is a frame. 44:02And that's what we got back to the frame. We had to significantly improve our thermal imaging. It was way, way too slow. And with a very, very. Poor quality. And the skull registration and the fusion between CT and MR took very long. It took like dozens of minutes, like 20, 30 minutes. And so we, I would say on one hand, it was a eureka moment because the team saw a focus spot in the brain through an intact skull.
Andreas Horn Yeah.
Eyal Zadicario But on the engineering side, we knew we had to go back to the drawing board and redesign a lot of the system components from scratch.
Andreas Horn Yeah. Okay. So, so what was the mood in the company?
Eyal Zadicario It was this, the, I think that in the very first one step was also a bleeding.
Andreas Horn Is that, is that, was that part of these three or was that later?
Eyal Zadicario No, it was later what happened after this really had no, no hemorrhages or bleeding. And there were, there were, I would say on that sense safe, but not effective enough. That's what we learned from these three. 45:00These three were, were, there were no safety aspects, but, but we just learned we were, we will now be able to really treat the tumor in a meaningful way with this, this type of system. So we went back. And you asked about the mood in the company. You know, as I said, we started this with a lot of skepticism, both internally in the company and outside the company. This only, this only kind of gave more, more, more emphasis that, that this may, this may not work. It may not be a way to drive enough energy to really ablate tumors in a robust way. So, so we went back and we redesigned the imaging, redesigned electronics. We built a much more powerful array. And basically, I think about two years later, something like that, two years later, we, we were ready to come with basically a platform that's much more, much more robust than, than, than that prototype. But we did have a decision point to make because there was, there was, there was a way to, there was a pathway to abandon this and say, Hey, it's not working.
Andreas Horn 46:02Let's, let's focus on what was then our commercial product.
Eyal Zadicario So, you know, from a company perspective, you always have these, these trade-offs of how much you pursue. And, and, and long-term, you know, vision of things that work and traded them off versus short-term progress and, and, and progress that you have to make. And it's still, still happening. It didn't happen back then. We decided not to abandon the neuro at the time. We saw the potential, but there were many voices that said we should shut it down and just commercialize, you know, fibers and stay with that. But, but we, we. These voices. These voices. These voices.
Andreas Horn Were these investors? Or colleagues or friends?
Eyal Zadicario Or was it also inside the company that many people said, let's shut neuro down or.
Andreas Horn Yeah.
Eyal Zadicario There, it was both. It was both. There was definitely a debate internally. You know, there's never like with, like with anything, there's never enough resource resources to do everything you want to do. 47:00Sure. Right. So, so how do you balance and, and there's in, in, in commercial companies, there's always a balance between short and long-term. And I would say InsightTech through the time has been able to leverage that and balance that well enough. So you have to get to a point where at the end of the day, neuro became our biggest commercial success. And really, I think drove FocusRestore sound to where it is today. So we basically bet on our scientific engineering teams to be able to overcome the challenges that that prototype had. So they went back and they redesigned the system with a, with a, with a probe that had now 1000 elements. That had new electronics that could drive four times the power. That. A patient. a patient interface that was much, much more tolerable. We improved the MRI imaging. We made the key algorithms much more robust and speedy. And it was a complete redesign of basically the system that's from the outside looks like what we have today. And in turn, obviously, progress has been made. 48:01And with that system, and what you asked about, with that system, we went back to the program. We went back to our GBM study. This was actually a low-frequency system at the time because one of the ideas to have more energy go through the skull was to lower the frequency.
Andreas Horn That's why we designed our lower-frequency helmet.
Eyal Zadicario Basically designed because the higher the frequency, the more the bone absorbs ultrasound. So the lower the frequency, the more ultrasound you get into the brain. And we went back with that system. We went back to the program with the low-frequency transducer back in 2007 and returned to that GBM study. And we treated one patient. That patient, a week after the treatment, had the hemorrhage that eventually led to him passing away.
Andreas Horn And we kind of took that as another kind of critical point to say, 49:01hey, then was this procedure related? How did this happen? And has this attributed to the low frequency?
Eyal Zadicario Because we didn't see that. It was a high frequency. And we got back and really evaluated how we can improve that and get back to the safety that we had in the original three patients before that. So again, another re-engineering cycle and rethinking cycle. But we also learned another thing that's important from a clinical trial design. We went to GBM patients initially because at the time, hemorrhage autofocus, ultrasound in the brain was very, very unique. It was new to the clinical research community. It was new to the FDA. And it was considered high risk from the regulatory perspective. Sure. And these types of challenges usually lead the study design to patients 50:01that have very few other alternatives to exploit in their disease progression or disease pathway. But GBM is a very, very, I would say, challenging target for specifically for ultrasound. First of all, they have their tendency to bleed even without a procedure. So there's some risk in bleeding regardless. They're very, very heterogeneous, very, very vascular, very, very, you know, I would say prone to mechanical effects and cavitation effects of ultrasound that make them very risky. And then at the end of the day, I think that's what led us to this unfortunate event. Again, unfortunately, we went through that. We learned a lot and we got back to the higher frequency with our new electronics. So we basically went back to the 650 kilohertz transducer, which was proven safe on the first three patients. But now with a brand new ExaBlade platform that is more powerful and more suitable for clinical need, 51:06and we kind of looked for a different target. And we kind of looked for a different target. And we kind of looked for a different target. And we kind of looked for a different target. Because we felt continuing to treat GBM with lesioning may kind of put this whole concept at risk because it's very, very heterogeneous, very, very prone to hemorrhages or bleeding. And we need a different target.
Andreas Horn Interesting. Okay. And maybe before we move to the different target, have you been to the Brigham at the time? Like, was there a team of Insight Tech present?
Eyal Zadicario I've just spent three years there. That's why, you know, I'm curious whether you had been there at the time as well or friends of yours. Yes, I've been at the Brigham almost as my home for those kind of five, six years. Spent a lot of time in Kulevo's lab. At the time at the Brigham, you know, you probably know Frank Joles, which was the kind of great visionary of focus ultrasound and many, many other image guided therapy at the Brigham. 52:05This was all done all in Kulevo. So I was in collaboration with them, our physicist team, our engineering team, me, myself, were there for the whole set of that study. A very, very tight collaboration between the Brigham and Insight Tech at that time.
Andreas Horn And the collaboration was probably, you know, your company from Israel doing this in the US, probably because of Kulevo's lab, right? Because they also had potential to, yeah, okay. Makes sense.
Eyal Zadicario So Kulevo was the great, you know, Kulevo's lab at the time was definitely the biggest focus ultrasound lab around. I would say it's two things. It's the Brigham being, you know, the fact that they were very advanced and innovative in your research at the time and still are probably.
Andreas Horn And the focus ultrasound expertise there were very, very great partners and great collaborators with us. So you learned from the glioblastoma that it is possible, right? 53:00But it's maybe not the right indication because of the cavitations and risk of bleeding and so on. How did you get to explore thalamotomy? Why, why?
Eyal Zadicario Basically around, so around 2006, I think we came to know a team in Zurich actually, that was doing thalamotomies for treatment of neuropathic pain. Actually with RF lesion, just like you're aware of. So they were doing bilateral lesions in the central medial and nuclei in the thalamus for pain. And we, they became aware of our technology. We came and presented it to them. And we said, look, we, we shared them with them our experience and they said, okay, that, that may be an even better way to do the thalamotomies that we do today. And not invasive, if you can do the non-invasively. And because of that experience and because we never did it before. And because as you're well aware, I'm sure this audience is well aware that the thalamus is a very, very sensitive and delicate area. 54:03You do, you really want to target only the nuclei you want to target. You cannot have. Any surrounding effects on the surrounding tissue or any effects on the surrounding tissue.
Andreas Horn But it is in the center of the brain, right?
Eyal Zadicario Which is. That's right. Fits well.
Andreas Horn Yeah.
Eyal Zadicario So it fits well, the technical need, but there's also clinical challenges that it comes with. Yes, yes, yes. You want to really, really be well, very well focused and very sharp in your focusing. So you're not getting any damage on surrounding tissue. So for almost two years we worked with them. On just testing the systems on ex vivo skulls and cadaver models and simulations that we ran and dozens of experiments that they ran in non-human settings on cadaver models and ex vivo skulls until around late 2008.
Andreas Horn Both teams felt that, yeah, we should, we should, we're ready to go and do the first thalamotomy.
Eyal Zadicario And that basically changed everything. 55:01I mean, September 23rd, 2008. It's a time to remember. For Foucault. Foucault SuperSound, you know, kind of history where the first non-invasive thalamotomy was, was done in a neuropathic pain patient. Two lesions, perfectly shaped, perfectly placed the same in the same treatment. It could easily seen on an MRI and with no adverse events or side effects to the patient. And we kind of felt this was maybe the biggest eureka moment of saying, Hey, now, now we've got it right. Because you could. You could actually, everything worked. I mean, the thermometry worked well. The lesion shape and location was, was perfect. The impact on the patient was perfect. There was no side effects. And I would say probably, you know, that eight years into this kind of said, okay, now, now, now we're onto something.
Andreas Horn Fantastic.
Eyal Zadicario It all seems like all I have goosebumps right now. So it all kind of came together. 56:00Right. So all the many struggles and valleys you had to go through, but now. This was the right indication. The technology was ready. The company was ready.
Andreas Horn Was this in Zurich or at Brigham?
Eyal Zadicario In Zurich, in Zurich. In Zurich.
Andreas Horn Okay.
Eyal Zadicario So this in Zurich was the first thalamotomy. You know, I would say Andy at the time, it was not obvious on the clinical side to take the risk and, and do a transparent lesion in the thalamus. Not, not, not that was very, very unique team that kind of saw the opportunity, had the experience with RF lesioning, which, you know, at the time was already kind of a, a losing.
Andreas Horn Yeah.
Eyal Zadicario It was a losing its momentum for, for DBS and, and, and went back and tried it. So their pioneering experience and our lessons learned through the hoops we had to go through, I think it was a perfect match on a perfect timing that sometimes you can't plan these things. They, they just happen. And, and really, really turn was, it was a, was most, really the most, the biggest inflection point in the neuro program when we naturally saw that first thalamotomy perfectly placed and not invasively. 57:04And this went on. And then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then, but then And I think you mentioned before that you kind of owe this to the Zurich team or like without them, this would not have happened. So you were really an oncology treatment company before this, I think. Right. Or can you talk about that a bit? You know, when we look from the way companies look at markets, you look at the market on neurosurgery. And, you know, there's two big things in neurosurgery. There's their vascular like stroke and other indications which are not so much lesioning. 58:03There may be room for that in the future for focus ultrasound, but we did not start there. And there's tumors. The neuromodulation part in surgery back 20 years ago was not very big. There was DBS, which was big and it was kind of upcoming and growing. But it was smaller from a market assessment perspective than tumors or vasculature. So we never thought we would do neuromodulation as a starting point. We thought we would do tumors and that will evolve into tumors and epilepsy and then potentially neuromodulation. By the way, neuromodulation from the way we saw it back then was the most challenging because the accuracy, the precision, the side effects in the thalamus, as you know very well, is very, very demanding. It's much more demanding than doing surgery on epilepsy or tumors.
Andreas Horn Yeah. And you see the tumor, right?
Eyal Zadicario 59:00Right. You might not see the tumor. Even the targeting is much more complex. So from the way companies look at markets, the way companies look at device development, it was not trivial that that should be the starting point. So it looked like at this time in history, September 23rd in 2008, that you were on your way to become a neuropathic pain company. But that didn't happen. That didn't happen because we tried to explore.
Andreas Horn Can we scale a market in neuropathic pain? And how is that patient population being treated today?
Eyal Zadicario And I would say the Flory team was a pretty unique setting that actually treated or had a neurosurgery program for neuropathic pain. Not too many neurosurgery departments had that. Neither the experience of lesioning for pain, nor how to scale a patient program around treating pain patients or neuropathic pain patients. 01:00:01Right. ! Right.
Andreas Horn thalamotomy look like? And he said, okay, what else can we do? What other indications can benefit from this capability?
Eyal Zadicario And at some point in time, the essential tremor came up as something that historically, and you know this very well from the many podcasts on this session that we're doing, when lesioning was performed before DBS, then movements were treated with thalamotomies at the time. And that kind of came back. So, and the people said, okay, that's a potential, but we don't recommend you go there because
Andreas Horn everybody's doing DBS now, and why would anybody 01:01:00go back to do lesioning?
Eyal Zadicario So, you know, most of the physicians at the time were not so, I would say, did not adapt going back to lesioning very, very easily. And also essential tremor was a patient population that, because of the invasiveness of DBS, were not the most commonly treated with DBS, mostly Parkinson's disease. So, essentially, go to Parkinson's disease. And we had to go through all this market assessment phase at that point in time. I think you mentioned that most people at the time told you that it would just be a handful of patients per center that could be done in a year, right, with essential tremor. So, there would be like five to eight patients per year or so, which we now know is not the case. But, that was what they told you back then.
Andreas Horn Yeah, because
Eyal Zadicario the essential tremor patient population is greatly disabled by the 01:02:00disease. And sometimes it has a huge dramatic effect on their life and their lifestyle and their disability. But, they choose not to go, and they take medication, which helps to a certain degree at a certain point in time. But, when they become therapy resistant, they chose not to go, or most of them, chose not to go through invasive surgery of either having an RF lesion or having a DBS. That was just what the fact was. Most of the patients were left untreated when they became drug resistant. So, there were very small volumes at the time in neurosurgery departments of actual essential tremor patients. So, that was the feedback we got, that it may take a very, very long time to run a study and get that approved. Again, the way things happen, 01:03:00fortunately enough, there was this team at the University of Virginia, which was led by Jeff Elias at the time, that said, hey, we will do this feasibility. It was a 15-patient study. And we decided to run and see, hey, let's see that one is effective and safe for essential tremor. And that we can actually recruit 15 patients. And it was not obvious. We estimated this would take probably two to three years, just based on the fact that the numbers you mentioned were the typical patient volume in these centers. But what happened, we started this study in February 2011, and by August 2011, the study was done. All 15 patients were done in like six months.
Andreas Horn Yeah, wow, okay.
Eyal Zadicario As soon as that study, that community became aware that there's a non-invasive solution for essential tremor, there was a big move towards getting on board 01:04:00in this study. That was another kind of big surprise. Another eureka moment that when you bring a new solution to an existing problem, you may find it maybe very, very helpful to patients that, until that time, just stayed without therapy.
Andreas Horn It's very interesting also tying back,
Eyal Zadicario to what you said in the beginning about, you know, creating a market. It can be unpredictable also in this way, where you underestimate the market because you would introduce something that's just easier to apply. You talked about this, like the, I think the whole,
Andreas Horn it has to be smooth, right? And if it's very smooth,
Eyal Zadicario it could be the market is much bigger than you thought.
Andreas Horn Is that correct?
Eyal Zadicario I think when you bring something that's fundamentally different from the patient experience that the patients know today, and you can think about anything that we use, not just in clinical settings, in every, in every setting. Sure. When you, when you have a product that's, that fundamentally changes the value proposition for the patient or the way the 01:05:00patient will receive their relief, then, then it can, it may also fundamentally change the market size and the market opportunity.
Andreas Horn Yeah.
Eyal Zadicario And sometimes it's, it's possible to predict that. And sometimes it's hard to predict that because I would say it was not a complete, uh, uh, you know, surprising the sense that we knew everybody knows that the patient population suffering from essential tremor is very, very large. People knew that we did not, we knew there was a potential for that. The, the, the, the, the, what we had to overcome is show that it's effective, show that it's safe and show that the patient experience is going to be significantly different than invasive surgery, that a much bigger patient population would opt to go, go get treatment.
Andreas Horn Yeah.
Eyal Zadicario It's, it's, it's almost like it's each, each, like we see this every, every day these days with,
Andreas Horn with, um, the focus ultrasound, uh, devices too, right?
Eyal Zadicario If, if a new clinic opens up shop, for example, Freiburg in Germany just had as a new device, 01:06:05I think since maybe half a year ago or a few months ago.
Andreas Horn And, uh, Falka Kooning told me the same story. They got many, many calls, right?
Eyal Zadicario Much more than for DBS.
Andreas Horn And, and there, there seems to be this kind of, um, first of all, it's, it's good. Marketing, right?
Eyal Zadicario It's incisionless and so on, but also there seems to be people that, as you say, would love to change their disease, but they, they would not want to have brain surgery in the classical sense. Right. And that, that is something, I mean, everybody, even starting from when Andres Lozano started advocating for it. Um, and then at the time it was still kind of new, uh, in the commercial sense. Um, he also said that it even sometimes drove the DBS numbers up because more people came into the clinic. Then got evaluated, right. But, but there was like, it seems to be, um, there's a, there's a big sleeping market, it seems right. Um, that nobody knows until you have such a device in a way, right.
Andreas Horn 01:07:04Um, yeah,
Eyal Zadicario Yeah, I think it was, it was two things that kind of think fundamentally changed the fact that you, that, that I'll call it for the patient's perspective, it looks and feels more like a therapy than a surgery because they don't feel like they're going through surgery. They're not going through anesthesia. They're not going through, there's no cuts. The effect is immediate. They walk out of the room and the tremor is impacted right away. There's no tuning or anything to do afterwards. And I think all these aspects together kind of drove this change in what we can actually offer patients. Super cool.
Andreas Horn What were our next steps? You mentioned the Virginia study. What came next? So you realized you were onto something, but what happened then?
Eyal Zadicario 01:08:00Since we had a lot of experience with other indications, we knew, we learned that we should make no shortcuts. And on one hand, we, for example, the way we designed the bigger study and the data collection, we said it's going to be a level one evidence, randomized controlled trial, went all the way to submit it in the New England Journal of Medicine, really made no shortcuts because we knew that adoption would actually be impacted a lot and the buying from the clinical communities and the professional neurosurgery society, their acceptance of that would just require the most rigorous study design, publication, and rigor we can implement. So we made no shortcuts. We did the right study design and the right, and the right publication to follow up with that. And I think that, you know, we knew that there's, 01:09:01in the neurosurgery society, there's people that are still aware of the benefits of lesioning for certain patients, certain patient population. You and colleagues like yourself that, you know, developed the noble art of lesioning and keeping that momentum of training new surgeons, of actually being aware, and knowing which patient can benefit from lesioning. We said, okay, that that'd be, that's just a new tool to a known modality that just, that would kind of really reinvent how we can bring this, this known clinical impact into patients. Super cool. And you did mention you published in New England Journal of Medicine, and I think it, this pushed out the acceptance of the, like the getting the paper out, long time, which we scientists suffer from already, right? For our careers, we publish these things and all that, right? But as a company, I would think, okay, if this takes a year longer, that's significant, right? Money-wise, or can you talk a bit about that, right? It's very significant. Yeah, very significant. And I would say, you know, it's not just the one year. So it goes back to my theme of data and evidence, 01:10:19So strong and rigor on data in the clinical setting, I think will always pay back. And so we had to wait after FDA for another year of follow-up with these patients because we wanted a real long follow-up for tremor. And I would say we then followed up for five years, these same patients, and published on five-year data. Because at the end of the day, both from creating a market requires this level of rigor. So there's no, I would say, no pushback on the fact that, hey, you may not have the right data or the right impact on patients. 01:11:04So the more you invest in good clinical study design, the more you invest in rigor and data collection, and the longer follow-up, at the end of the day, it pays back. But as we mentioned earlier, it's a trade-off because it takes more time. There's no way to shorten the follow-up.
Andreas Horn And time is money for you, right? Yeah, just to even pay employees and everything. Yeah, yeah, okay, yeah.
Eyal Zadicario So we started commercializing as soon as we got FDA approval, but we knew that until we get the three-year data and the five-year data and the reimbursement that requires that level of long-term evidence and outcome, it would be hard to scale.
Andreas Horn And that's why our earlier years were challenged by that.
Eyal Zadicario We had to just wait for that to happen. Got it.
Andreas Horn Okay. Did I understand it right that FDA approval and reimbursement was tied to this being like the long-term follow-up? Interesting. Okay.
Eyal Zadicario The regulatory approval came in, I think, mid-2016, 01:12:03but that required a three-month follow-up to get FDA approval. We waited a year to publish because we wanted to publish in the New England Journal of Medicine. That required a one-year follow-up. And then for reimbursement, again, different levels of reimbursement required more follow-up until we had this five-year data, which is the last we published.
Andreas Horn Okay.
Eyal Zadicario So this was the feasibility trial, probably one of the most pivotal things in the history of MR-guided focused ultrasound to show, you know, publish in such a prestigious journal like the New England Journal, show it's feasible.
Andreas Horn But after that, there's a roadmap to commercialization. What was that?
Eyal Zadicario So I think the roadmap to commercialization goes through, first of all, I would say the technicality of getting approved and getting it covered by either private insurers and then national coverage. 01:13:02Each country has its own, you know, mechanics of how you get that done and processes. Some are longer. Some are shorter. Some allow you to leverage kind of other country evidence or global evidence. Some require local. Some require local evidence or local guidelines or vetting by local societies. So then you start in a pathway where in each of your key markets, you have to go through that process. And we did that pretty quickly and in a few years got it reimbursed in the key markets. But I would say in some regions in Europe, we're still struggling with it. We still need to get that done.
Andreas Horn So it's a work in progress that takes a few years. What changed of how people think of leasing with this?
Eyal Zadicario I think, as you mentioned, that was one very, very pivotal moment when that was published in the New England Journal of Medicine. And then, you know, better than anybody, the society back then, the neurosurgery society, 01:14:01all the movement is all those specialists, especially around the functional neurosurgeons, were all around DBS, which has a lot of benefit for many, many patients. And I would say changing the model. The mindset of they would they would call it going back to leasing. We thought it like going back. It's actually going forward because the way we do leasing is nothing like has been done, you know, in the early sixties or seventies because it's not just the focus ultrasound that invasive. The fact there is no tissue shift, the probe, the fact that it can be, I would say, localized and move in real three dimensions, not just along a trajectory of the tract if you need to readjust or pivot. But actually, we position this as leveraging other advancements in MR imaging of actually 01:15:02doing functional imaging and functional mapping and later tractography to actually have a much more personalized lesioning technology than in the earlier decades. I mean, you know, the earlier decades when we had, we really did not have any personalized lesioning. The lesioning we can do with focus-refer sound has two fundamental ways of how we personalize it. First, it's the imaging that's advanced a lot since then, since the early days. First of all, MRI anatomy has gotten much better. DTI and tractography had a lot of capabilities to actually personalize the target based on the individuals. And MRI images and not just go by stereotactic coordinates or adapt the basic stereotactic coordinates per patient. But on top of that, which is very unique for ultrasound, we do this, I'll call it stimulation 01:16:00sonication before we actually ablate the tissue, which with RF is more difficult to do or not doable because we can actually do a small. And then we can actually do a non-lesional thermal rise of three, four degrees, which has some transient effect on the tremor or side effects if you're off target a bit. And you can actually not only personalize the targeting based on feedback you get from the patient, you also can actually see the lesioning happening in real time and sculpture it and move it and actually around in 3D space to personalize and personalize the lesioning. And that's really, really important. And I think that's really important. And I think that's really important. And I think that's really important. And I think that's really important. And I think that's really important. And I think that's really important. And I think that's really important. And I think that's really important. And I think that's really important. 01:17:11And I think that's really, really important. was a completely different way of doing lesioning compared to the past yeah i mean even you like hearing you speak about it now and thinking about all the technologically complexity to get there and get it and get it done it's really it's remarkable you can test sonicate but you can also see where you test syndicated you get sculpted around maybe in the future even even more right like you could imagine algorithms would help you shape it around or you know yeah there's so much um already done but also that could be done with this technology so um
Andreas Horn really fantastic what do you think like speaking about the future of
Eyal Zadicario fuss what do you think are the next challenges or next opportunities of the field yeah so i think you know insetex achieved a lot in positioning focus ultrasound in a way that i 01:18:03think now in the brain but not only in the brain i think it's a modality that has a role in in in medical care i think many have tried before and we've been persistent enough and and lucky enough and innovative enough whatever and to really i think now there's there's definitely a role for ultrasound in therapy in general and in in in the brain specifically so today i think that does focus ultrasound have a role in in health care i think it's just the question should be how big and where is where is that role it's not it's not an if anymore yes i think that if you look at kind of our or we started this in 1999 or this was more a science project with a huge potential i think now it's a reality and we can just debate on how big the potential is and where the shortest improvements that can be but i think i think we've crossed that barrier is there a role i think there is a role just a question of how big 01:19:01how big it is and how fast will the market adapt it i think that that's that's our next challenge and i i think um so so i heard this at the at a at a conference that that um last year or even before focused ultrasound has been the main treatment modality for essential tremor overtaking dbs and other modalities um do you do you see maybe similar growth curves for other disorders or new indications even that you might be exploring these days that that that could you know overtake other forms of treatment first of all for essential tremor it's absolutely right and the thing that we we see that number growing every year i think that you can just say we probably 2024 last year we treated more essential tremor patients than any other surgical modality as you mentioned and i think that we will probably treat in the 01:20:04following years even more and more that's that that's growing all the time um i think that the movement disorders you know we now we are also approved for parkinson's disease uh in most of the world i see this more in general as a complementary tool i i we don't have a claim that this will treat every patient there's definitely benefit in the in the other treatment modalities and dbs and others and medication for certain patients but there are certain patients that need a or would be best served by by envisioning a treat by envisioning a treatment of what we can do. So I think for us, it's growing the awareness and awareness within patients, awareness within physicians, awareness within the community, awareness within insurers of actually, you know, making this therapy as an option to every patient that can benefit from that. 01:21:01And I think there's more and more for us to learn how we actually improve and increase that patient population that can benefit from the technology.
Andreas Horn Fantastic.
Eyal Zadicario You recently launched the ExaBlade Prime.
Andreas Horn What did it bring? What's new with it? It still has a frame or not? Yeah, it still has a frame.
Eyal Zadicario It still has a frame. Basically, the frame is there mostly because we need the head really, really stable during the procedure because we're making, this personalized targeting where you move the spot by a fraction of a millimeter, which has an impact in the thalamus, needs the head to be very, very, very rigid and precise. So we don't want to move that during the procedure. So from, you know, almost a decade now since our first approval in 2016, we improved a lot 01:22:01and we learned a lot from our customers, from our patients, from the feedback we get from the users. And the most, the biggest thing we're focused on is how to continuously improve the patient experience. And the patient experience, I mean, preparing for the treatment, during the treatment, after the treatment, and making the treatment as short as possible, as tolerable as possible, reducing side effects. That has to do a lot with what Andy, you mentioned earlier about spot shaping and spot targeting and how we use all the personal information to actually improve the patient experience. We believe that if we continuously improve the patient experience, meaning less side effects, shorter treatments, better efficacy, then this is the key to our progress and success. And just bring this and do better for those patients. So really, really focus on improving the patient experience and the rest will follow. 01:23:00Prime is our newest, the product release, because this is a version that we worked on for the past five years almost. It basically took the data from the first six or 7,000 patients we treated between 2016 to 2019, let's call it. And did a lot of learning from our users, from the workflow. And that data was fed to multiple, to multiple, machine learning algorithms to actually improve and automate a lot of the things that we used to do, or physicians used to do manually. So predictive models for the right parameters for each patient, the best parameters to overcome the skull focusing, integrated tractography as a treatment, as an input to the treatment planning phase. We baked all that into a workflow that's much more optimized. If the first treatment back in the, I'll go back to the first, first treatment, 01:24:01these took like hours. Right. Three hours, four hours, sometimes five hours. Today, typical treatment in the commercial settings takes an hour and a half. Wow. So all these improvements are not only the technology, the physicians getting trained and getting confidence in the system, but there's a lot of progress, a lot of manual things that were done and were very tedious and time consuming that became automated and with a lot of assisting tools, for the physicians for their decision making. But I would say that it's a huge step up from our previous versions. Probably our first, I would say fully commercial product version that took all the inputs from five years of working in the field into a really most advanced product that we have. And there's still more to do. We still learn a lot from our current users. 01:25:01The more we do, the more we learn. We survey the customers, we survey our user, our patients. We try to learn what will get us to our ultimate goal. And our ultimate goal is that, is that the patient experience will be such that every patient that can benefit from a treatment will actually get it.
Andreas Horn Yeah.
Eyal Zadicario That every physician will feel comfortable and for the right patients, it's the right treatment that would not hesitate. And it has to do with improving our side effect profile and making it a shorter treatment and making it more tolerable. And there's a lot more to do on that. Of course. We talked about the frame and the pins. We're still asking for the patients to shave their hair before the treatment. We want to get rid of that at a certain point in time. So there's still a lot of things there to do to get to our ultimate goal of making really, really outpatient friendly and physicians' preferred choice for patients that can benefit from it.
Andreas Horn Fantastic. What's in the future beyond movement disorders?
Eyal Zadicario 01:26:00So I think that's a big question. I think there's the way we look at the future for us and for focused ultrasound in the brain, there's various aspects. And there's a lot of, I would say, I'm proud that we put the technology at a point where physicians feel confident enough to do site initiated studies and explore other things. And there are studies going on for unique indications that can benefit patients. And there's a lot of research going on that can benefit from lesioning in the center of the brain. One target is for epilepsy that's been published
Andreas Horn and other targets, some are still studying neuropathic pain. And this may evolve to a much bigger opportunity.
Eyal Zadicario And I think that one venue is the thermal lesioning
Andreas Horn and where else can we do that in the brain?
Eyal Zadicario The other aspect of where this can go in the future is non-thermal lesioning. That is now being recently approved for liver tumors 01:27:03or liver treatments with histotripsy. There's definitely a potential for such therapy in the brain as well. I think we're years away from that, but I think it may open up other opportunities for targets that we cannot reach with thermal ablation just because of the physical constraints of driving enough energy to the target. I think at whole, our vision would be that in neurosurgery, there would be an acoustic neurosurgery platform that can actually treat any surgical target, not invasively, just harsh stuff, no radiation, no incisions.
Andreas Horn And there would be a day when we would say, why did we cut the body to destroy that target?
Eyal Zadicario There are non-invasive ways to destroy that target that are safe and effective. And that's what we've shown in the VIM in the thalamus. And there's other targets that can be used. There are other targets that can greatly benefit from such a vision and a technology. 01:28:02You mentioned there will be a day with an acoustic neurosurgery suite. I think when I talked to Kulervu, and I had to have nudged him to talk about the distant future, he said everybody will have a device at home.
Andreas Horn Would you go that far?
Eyal Zadicario So I think there's definitely... So I talked about the surgical pathway, which is, I would say, the most... I won't call it near term. I think it's within reach. I think outside of that, you touched upon two things, and what you mentioned, Kulervu, is all kinds of, I would call, non-surgical uses of focus ultrasound, be it neuromodulation, be it blood-brain barrier disruption. And I would even go as far as the vision of brain mapping that you could study. I mean, I envision a day where this is safe enough, that you can, just like you study healthy volunteers 01:29:01in MRI imaging, because you think MRI is safe enough, then there will be a day when we can use focus ultrasound for brain mapping, for either localizing a disease or diagnosing a neurological pathology without visioning, just by neuromodulation. And I think the... the vision of home care with focus ultrasound for neuro or other aspects, especially in the neuromodulation domain, I think is probably doable. It'll require a lot of understanding, not so much the technology, by the way, or more the understanding of the right targets, the right parameters, and the right disease states, where to utilize that. But I see that we've crossed the line, and we've crossed the barriers I mentioned earlier between focus ultrasound being a vision 01:30:00and a science project, to being a treating modality or a treatment modality that can be used in multiple ways. Surgical and lesioning is one of them, maybe the first and the most obvious. You know, we made a lot of progress on blood barrier disruption as well, to deliver drugs into the brain. And I think we all know neuromodulation is the next big thing. That can start in a clinic setting, can move to home care. I think we all see pathways to make that happen. Super cool. Just talk to Leonard Verhagen,
Andreas Horn who you may know, of course, in Nijmegen, and he mentioned for the functional uses, so you talked about brain mapping, right?
Eyal Zadicario Looking at, for the listener, this would be like trying with ultrasound to look at what the brain is doing, the brain activity mapping, like fMRI is doing at the moment. This is a very active field of study, certainly in animals, but even I think in humans, 01:31:01theoretically possible, including with the intact skull. But I think so far uses injections of microbubbles, lipids, something, a contrast enhancing. But he mentioned that it could be theoretically possible without that, even in the future. I think it needs a lot of like it's more a computational problem rather than a...
Andreas Horn Is that true? Is that accurate?
Eyal Zadicario I think it's a computational problem and that will, again, eventually will overcome that. I think computational power is, you know, becoming higher
Andreas Horn and better every day.
Eyal Zadicario I think, why do I believe
Andreas Horn focus ultrasound has a unique role in that?
Eyal Zadicario Because it goes back to the basics of what we were able to do today focused ultrasound in the neuromodulation phase, in any location in the brain, we can do that non-invasively, we can do it very precisely. 01:32:00We can actually stimulate more than one target at a time or the sequence of stimulation that no other invasive modality can do. So if you want to actually, and I think where neuromodulation will go, is that you need to, I think it's not going to be like in oncology or even in what we do with functional surgery today. Neuromodulation is going to be much more about circuits than targets. So what other modality, if you think of a modality that you want to stimulate in a certain pattern, in a certain timing, for example, circuitry in the two hemispheres or circuitry along various neural network, then focus neural sound can do that because you can rapidly steer, you can steer it anywhere, and you can stimulate multiple targets either simultaneously or in a certain sequence of timing to either study or replicate or diagnose a certain pathology. 01:33:01So I think there's so much to do there that the computation power will obviously grow to a point where we'll see focus ultrasound really play a role in a way that no other modality can actually do non-invasively.
Andreas Horn Yeah, yeah.
Eyal Zadicario And there are many startups also popping up these days in this field, I think. It's very exciting to think about the future.
Andreas Horn And yeah, I really like your acoustic surgery suite
Eyal Zadicario where you can do all of these things. You did mention blood-brain barrier opening. That is, I think, widely known by now, the idea where you open it
Andreas Horn and then a drug can perfuse, enter the brain locally, not everywhere, right?
Eyal Zadicario So for example, to treat a tumor, or other disorders. Very fascinating concept. I think a little bit lesser known would be the inverse of that to essentially take a biopsy by opening the blood-brain barrier locally
Andreas Horn where you are interested in what happens there 01:34:03and then things from the brain can enter the bloodstream and you can take blood and measure it, right?
Eyal Zadicario So these two things, although very similar, one is more for treatment, one more for diagnostics.
Andreas Horn Can you give an overview, or state of the field of these two things and what the developments are, who the key players are, the successes and so on?
Eyal Zadicario Yeah, so I think that that's... We started with blood-brain barrier opening and it was studied in preclinical settings for many decades. And I think there was always a promise that if you can deliver drugs or any other agents, call it gene therapy, viral vectors, drugs, you can do it. But if you can deliver drugs into the brain more effectively, then that would have a huge impact on certain diseases, mostly oncology, but not only oncology. So we adapted our platform to allow blood-brain barrier opening. 01:35:03And we've probably done hundreds of sessions by now in multiple studies and executions. We're seeing great, promising results in that domain. I think it's pretty well established by what we've published and what others have published that... The fact that we can demonstrate localized and transient EVP disruption is well established. I mean, it's, again, beyond the fact that, yes, you can safely and effectively open up a barrier. It took, you know, not more than a few years for the community at large to kind of accept that. Many published around that, with our technology, with other devices. And I think now it's more in the research of the right drug, the right disease, the right dosing, and there's multiple studies and startups and other companies following that pathway. And I think, again, you can look at this more broadly and say, the fact we're opening up... 01:36:00Again, it's the only modality that can do that. Ultrasound is the only modality that can locally and in a transient way disrupt the blood-brain barrier. And nobody, no other modality can do that. Now that on its own changes the dynamics of how the body reacts to that. You know, there were originally few studies that showed that even that on its own has effect in certain diseases because you are helping the body do something it could never do before. So there's a pathway there. What to study further, what does just brain blood-brain barrier disruption, even without a drug, can actually do for certain neurodegenerative diseases like Alzheimer's or ALS or others. Now, on top of that, you can deliver agents and you can, you can deliver drugs that are known today to not penetrate the blood-brain barrier and make them more effectively locally, or even reduce the overall doses and toxicity in other parts of the body. That's what usually happens today. You increase the toxicity to make, to get enough drug into the brain. 01:37:04But you don't need to do that if the blood-brain barrier is disrupted or opened at the target region. And maybe the future of that is actually delivering, I would say, more biologically targeted, I'll call them agents like gene therapy or immunotherapy drugs that are actually optimized for certain gene or certain oncology, pathology to treat and deliver more effectively into the brain through disruption of the blood-brain barrier. And there's multiple, you know, ways to do that. I think the fact that it can be done noninvasively is pretty well established today by what we've studied and exported, what others have shown. Again, our technology today, we run it in various trials. One of them is, as you mentioned, is in the diagnostic setting 01:38:00of actually opening up the blood-brain barrier to get a tumor, DNA information into the blood and getting that analyzed to make much more proper disease management decision-making by clinicians. And, and, and,
Andreas Horn Fantastic. Can you maybe just briefly touch upon sonogenetics, maybe even for the listener, briefly tell what it is and whether you see a future of this?
Eyal Zadicario 01:39:00So, sonogenetics or sonodynamic therapy actually, you know, evolved from photodynamic therapy, where certain drugs get activated by the ultrasound. So, certain drugs are activated by light and you use laser to activate the drug, but you can also use on certain drugs sound or the pressure wave to actually activate the drug. And there's various studies of that with our platform as well around agents that can be delivered systemically. They get to the tumor, but the ultrasound activates them only at the tumor site. And there are certain initial evidence that that has been...
Andreas Horn Yeah.
Eyal Zadicario Very, very promising in certain oncology settings, DIPG and others for young patients. And we're following that as well. Again, it's one of those areas that ultrasound is the means to deliver the 01:40:06therapy. It's not actually doing the therapy, it's the drug that's doing the therapy, but again, it's the only way to do it invasively.
Andreas Horn Yeah.
Eyal Zadicario Yeah. Because otherwise you'd have to put some light sources or laser.
Andreas Horn Yeah.
Eyal Zadicario Or some other light source into the target to activate the drug. But the wonderful thing about ultrasound is that it can activate it non-invasively.
Andreas Horn Very interesting. Yeah. Okay. I want to be respectful of your time. Just a few rapid fire
Eyal Zadicario questions to wrap up. This was super enlightening already. Do you have any advice for young,
Andreas Horn maybe even researchers, academics that want to enter industry? Or other people that want to start their career in industry? Any young people advice?
Eyal Zadicario First of all, I must say that the great thing about the ultrasound societies and meetings that 01:41:00you see so many more young people today getting into ultrasound, by the way, both on the clinical side and on the scientific side, you see people, young people today coming out of fellowships and
Andreas Horn saying, hey, yeah, I'm going to do lesioning for these patients because lesioning is back. And we
Eyal Zadicario didn't see that. 15, 20 years ago. That's great to see. In terms of advice, you saw the pathways. You got to be persistent with what you believe in. There's a lot of hurdles and a lot of groups to go through. But I think it's just, I would say my listeners that the rigorous work and pays off at the end of the day. I think you want to do something meaningful for patients. It may not come at the first first shot, it may not be quick, but when you get there, it's really worthwhile.
Andreas Horn Fantastic. Any missed opportunities we have as a field, right? Things we should
Eyal Zadicario be doing but are not doing enough. And I mean the entire field of neuromodulation, but could 01:42:03be for, yeah. Focus on. For neuromodulation, I think that the, I think the field will evolve a lot with this being noninvasive. I think this field has been very invasive. It's going to be either recording electrodes, lesioning or treating electrodes. But the fact that you bring to this whole field of neuromodulation, a noninvasive tool, I think will just unleash so many opportunities that I can't even, you know, think of. I think you just need to study that with the neurology community, with neurosurgeons, with neuroscientists. And the fact just the advancements in both imaging, understanding of the body, and the ability to do that. I think that's a very important thing.
Andreas Horn Yeah.
Eyal Zadicario 01:43:04. Final question I should have asked. I think we covered everything. And I think this series of podcasts that you put is very, very instrumental in neuromodulation in general. I think it brings to, I would say, younger adult history, which is so important. It falls over so many decades with so many lessons learned. I mean, I shared mine, but I'm sure the others have shared theirs. And there's so much to learn from. And, you know, at the end of the day, I think understanding the brain, that this century of brain understanding is just ahead of us. And I think it's just going to be a lot of innovation going that way.
Andreas Horn Fantastic. So thank you so much, Eyal, for taking the time off your busy schedule.
Eyal Zadicario And I hope you get to enjoy the beach a bit these days. I have to say it because I see it and I envy you a bit there in Haifa. 01:44:01And we'd love to meet, you know, at SCAM conferences. And thanks again for taking part. Thank you. I really appreciate you taking the time and giving me the opportunity.
Andreas Horn And also for carrying this podcast, which is really, really great.
Eyal Zadicario Thank you.
Click any highlighted text passage to jump the Spotify player to that point. The transcript text is present directly in the page HTML for search engines and accessibility.